Case
A 28-year-old woman of Nigerian ethnicity was referred to a dermatology clinic for management of facial skin hyperpigmentation. Her referral was based on the persistent nature of acne and postinflammatory hyperpigmentation (PIH) that had been present since her early 20s. Her acne flare-ups were not associated with her periods, which were regular. Her sister had cystic acne. Prior to referral, she had not trialled any prescribed treatment. She applied African soap, olive oil and shea butter as emollients on her hair and scalp to smooth and lubricate her thick, tightly curled hair to be more manageable and amenable to styling. The use of such hair products is common among those with Afrotextured hair.
Examination demonstrated hyperpigmented macules and papules, and open and closed comedones over her forehead (Figure 1). There was no involvement of her chest or back. There were no nodules, erythema, scale, plaques, excoriations, follicular accentuations or hirsutism. Incidentally, recession of the anterior hairline was noted suggestive of traction alopecia. This was secondary to tightly pulled hairstyles used in the past, including braids and weaves.
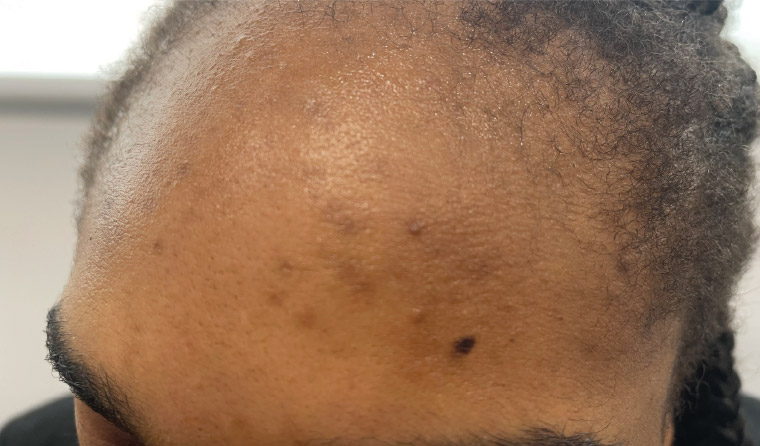
Figure 1. A 28-year-old woman of Nigerian ethnicity with hyperpigmented macules, papules and comedones over her forehead.
Question 1
What would be your differential diagnosis in this case?
Question 2
How would you manage this case?
Answer 1
This patient’s age, history of acne, use of occlusive hair and skincare products like shea butter and olive oil and the presence of papules and comedones limited to her forehead suggest acne pomade with secondary PIH. Acne pomade is the name given to acne that results from the application of occlusive products on the hair and skin. Darker pigmented skin are more prone to PIH due to predisposition to systemic inflammation and differences in molecular organisation and cellular activity between lighter and darker pigmented skin.1 There is a tendency for visible hypermelanosis to last longer and be more apparent in skin of colour.2
However, it is reasonable to consider alternative differential diagnoses, such as Malassezia folliculitis and rosacea, which can also present as inflammatory papules with dyspigmentation in a young woman. The key differential diagnoses in this case are presented in Table 1.
| Table 1. Differential diagnosis in this case, including relevant positive and negative clinical findings |
| Differential diagnosis |
Relevant positive findings |
Relevant negative findings |
| Acne pomade |
- History of acne
- Clinical features: Open and closed comedones
- Distribution: Forehead
- Genetic factors: Sister with cystic acne
- Environmental factors: Regular use of oil-containing skin and hair care products3
|
|
| Malassezia folliculitis |
- Commonly associated with acne vulgaris
- Distribution: Face
- Clinical features: Monomorphic papules4,5
|
- No polymorphic lesions
- No use of corticosteroids or antibiotics or immunosuppression4
|
| Rosacea |
- History: Dry, flushing, skin sensitivity or burning sensation; triggers include spicy food, heat, alcohol, gritty feeling in the eyes
- Clinical features: Background erythema, pustules and papules,6 eyelid erythema, conjunctival injection, crusting, recurrent hordeolum or chalazion. Might have oedema of the skin
|
|
Answer 2
This patient’s main concern was her PIH, which is a common complication of acne in patients with skin of colour. It should not be ignored. A multimodal approach is required for the treatment of PIH and its underlying cause through lifestyle modifications and pharmacological and procedural therapies.
Because the patient is yet to trial any therapies, general measures should be suggested first. Photoprotection through the use of broad-spectrum sunscreen (SPF 50+) and protective clothing, such as hats, will reduce further darkening of the affected skin. Avoiding skin irritation, such as from scratching, rubbing or irritating fragrant skincare products, is also important.7
However, to best treat the PIH, the acne must also be treated. The patient should be educated on how the use of occlusive hair oils and pomades contributed to her acne and encouraged, in a culturally sensitive way, to stop using these products.8,9 She should be encouraged to use oil-free, fragrance-free, non-comedogenic cleansers. An example of a culturally sensitive approach would be to try to learn about the hair care practices for this patient and to provide alternatives to oil-based products, such as silicone, along with practical recommendations for washing her hair weekly or fortnightly with clarifying shampoo. If oil-based products are the only ones this patient wants to use, she could consider application 2–3 cm away from the hairline with a covering over the hair at night to prevent indirect spread to the skin.
Topical tretinoin and adapalene are commonly prescribed retinoids in Australia for both acne and PIH. Due to the irritant potential of all retinoids, low concentrations should be used initially, with application starting a few times per week and gradually increasing as tolerated.7 This can be combined with the extraction of comedones. Benzyl peroxide and topical antibiotics could also be combined with retinoids for this type of acne. If the acne does not demonstrate improvement over a period of approximately eight weeks, oral antibiotics could be considered. Oral isotretinoin (dermatologist referral needed) might be required for severe cases that are not responsive to topical therapy alone and in which triggers are unable to be completely eliminated.
Because PIH was the patient’s primary concern, additional treatment measures can also be offered. These include topical hydroquinone, azelaic acid, chemical peels and laser-based treatments (Table 2).
| Table 2. Key considerations for treatments of postinflammatory hyperpigmentation |
| Treatment |
Considerations |
| Topical therapies |
| Hydroquinone |
- Application to the entire face is preferred over spot treatment for multiple areas of involvement to prevent irregular pigmentation because hydroquinone reduces pigment in both normal and hyperpigmented skin
- Risk of a temporary halo of hypopigmentation in the periphery of treated areas that can take months to resolve after treatment has stopped
|
| Retinoids |
- Risk of exacerbating PIH (by causing erythema) if used too aggressively
|
| Azelaic acid |
- Localised burning or stinging on the skin as a common side effect
|
| Hydroquinone–retinoid–corticosteroid |
- Combination hydroquinone and retinoid with a steroid component to reduce irritation potential
- The steroid component might worsen acne
|
| Chemical peels (eg salicylic acid, glycolic acid) |
- Chemical peels up to certain concentrations are available over the counter in various formulations, such as cleansers
- Can aggravate PIH after application
- Higher risk of side effects in skin of colour
|
| Laser and energy-based devices |
- Bespoke settings with lower energies are required to avoid medium- and long-term complications like scarring and permanent dyspigmentation
- Patients need to understand that multiple treatments over several settings are the best approach to avoid adverse outcomes in PIH in patients with skin of colour
|
| PIH, postinflammatory hyperpigmentation. |
Case continued
The patient was diagnosed with acne-associated PIH, likely contributed to by hair oils and oil-based creams and conditioning treatments. She was prescribed a hydrating cleanser, emollient and topical tretinoin and advised to opt for oil-free, non-comedogenic skin-care products.
The patient was discharged back to her general practitioner to monitor progress with a plan to review further if the initial measures were not successful.
Key points
- Recognise the importance of treating PIH in skin of colour, because it can be a significant patient concern.
- Inquire about cultural practices that might contribute to acne.