Case
A six-year-old boy with skin of colour presented to his general practitioner with a 1.5-year history of slowly progressive white spots on the skin of his face. The first lesion appeared underneath the right eye. He was subsequently referred to a dermatologist for further evaluation.
There were no significant features in the past history or family history of vitiligo other than his mother being diagnosed with autoimmune thyroid disease (AITD). On examination, there were multiple 5- to 10-mm well-demarcated depigmented macules present on the forehead (Figure 1), eyelid and upper malar region (Figure 2), trunk, axillae and right knee. There was no evidence of scale or erythema on the face or body, and no postinflammatory hyperpigmentation was seen.
A diagnosis of vitiligo was made, and the patient was screened for associated autoimmune comorbidities. Topical tacrolimus was used twice daily to attempt to repigment the areas of vitiligo on the face, whereas ultrapotent topical steroids were carefully used cyclically for affected areas on the body. Complete repigmentation was noted on his face and near-complete repigmentation was achieved in affected areas on the body after four months.
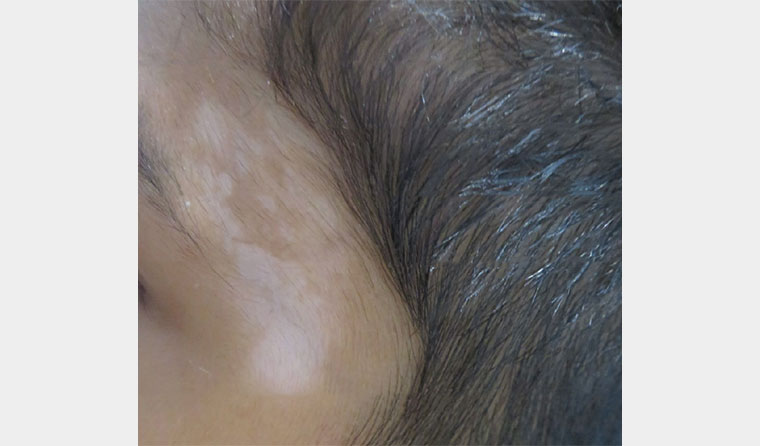
Figure 1. Vitiligo lesions present on the forehead.
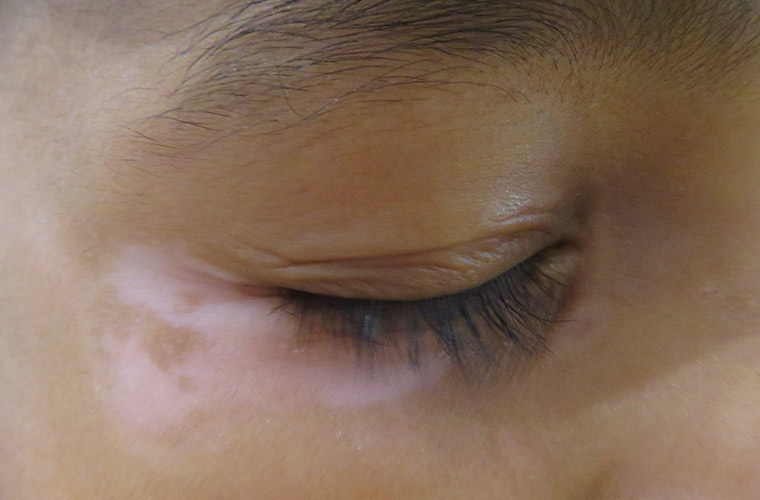
Figure 2. Vitiligo lesions present on the eyelid and upper malar region.
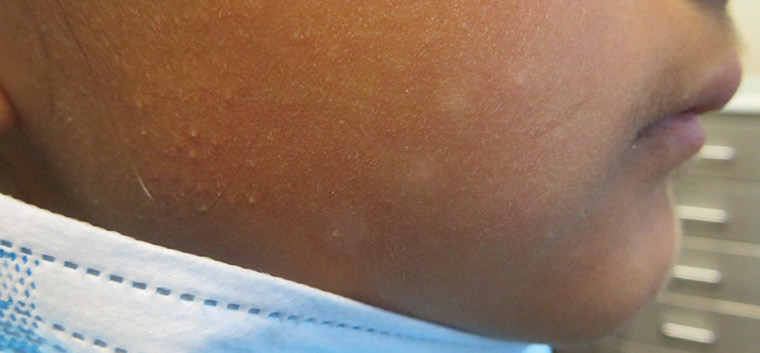
Figure 3. Pityriasis alba lesions present on the cheeks.
Question 1
What are the clinical features of vitiligo?
Question 2
What are the possible differential diagnoses?
Question 3
What is the treatment of vitiligo?
Answer 1
Vitiligo is one of the only acquired causes of depigmentation of the skin, with an estimated prevalence of 0.5–2% worldwide.1 It is an acquired, chronic depigmenting disorder resulting from the autoimmune destruction of melanocytes.2 Most other conditions causing depigmentation of the skin are congenital in nature.
Differentiating hypopigmentation from depigmentation is the key to navigating the differential diagnoses of acquired causes of white spots on the skin. This can be achieved clinically in the vast majority of cases. Hypopigmentation appears as poorly demarcated, slightly lighter areas of skin, whereas vitiligo is seen as well-demarcated, stark white macules anywhere on the face, body, genitals, mucosa and/or hair.
Koebner phenomenon is associated with vitiligo, whereby trauma to the skin can trigger new lesions.2 Koebernisation can be seen in acute lesions of trauma, but might also be seen around old scar sites, evident in the form of white scars in areas of prior surgery or injury. A total body skin examination of the patient should be performed to look for other areas of involvement, for evidence of leukotrichia (white hairs) within affected patches and for evidence of halo naevi (a naevus surrounded by a white ring) because this might precede the development of vitiligo.2
A Wood’s lamp can also be used to identify hypo-/depigmented lesions in those with lighter skin types and can help rule out other differential diagnoses. Evidence of an underlying primary dermatosis such as eczema might help give clues to diagnoses such as postinflammatory hypopigmentation if the white spots are only subtly lighter than surrounding skin.
There are two broad categories of vitiligow:1 a non-segmental variant, which is the more common type, involving many areas of the body; and a segmental variant, which follows a dermatomal-type distribution and is seen in approximately 2% of those with vitiligo.3
Vitiligo is associated with over 65 other autoimmune conditions, including AITD, Addison’s disease and type 1 diabetes.4 Work-up should always include an AITD screen given the increased risk of developing this condition, with AITD occurring in 15% of those with vitiligo.5 There is a higher risk of developing AITD with longer disease duration and greater body surface area affected.5 An initial thyroid-stimulating hormone level should be ordered and referral to an endocrinologist considered if the patient is hypo-/hyperthyroid. Other autoimmune diseases are not as common and thus should only be screened for based on reported symptoms and clinical suspicion.
The psychosocial impact of vitiligo is well recognised given the disfiguring nature of the condition. Patients might also present with associated psychiatric symptoms, including lowered mood and self-esteem.6 Given the association between vitiligo and increased risk of mental health associations, patients should be screened for comorbidities such as anxiety and depression, and treated if required.7
Answer 2
The most common differential diagnoses in this case are described in Table 1.
| Table 1. Differential diagnosis of vitiligo in this case study |
| Differential diagnosis |
Description |
Distinct clinical features |
| Postinflammatory hypopigmentation |
Hypopigmentation that occurs following an episode of dermatitis or inflammation |
- Poorly demarcated depigmentation
- More common in patients with skin of colour
- History or presence of a rash/itch preceding the white spot
- Evidence of a primary dermatosis might be seen
- Gradually fades over weeks to months
|
| Pityriasis alba (Figure 3) |
A benign, self-limiting form of atopic dermatitis that is more common in children with skin of colour |
- Mainly affects children and adolescents
- Poorly demarcated areas of scaly hypopigmentation commonly on the face +/– arms and forearms
|
| Tinea versicolor |
Due to overgrowth of yeast Malassezia spp. |
- Scaly area of hypopigmentation
- Normally around the trunk
- Usually seen in warmer climates due to increased fungal growth with sweat
- Positive microscopy
- Fluoresces yellow–green on Wood’s lamp
|
| Iatrogenic hypo-/depigmentation |
Examples of iatrogenic causes of hypo-/ depigmentation include:
- use of topical or intralesional/intra-articular steroids
- lasers and energy-based devices
|
- Hypopigmentation or depigmentation at the site of treatment
- Usually fades with time (unless severe laser injury)
|
| Leprosy |
Chronic bacterial infection of Mycobacterium leprae |
- Chronic depigmented skin lesions
- Endemic in particular tropical countries/regions
- Associated numbness or altered sensation of affected skin
- Positive microscopy
|
| Mycosis fungoidesA |
Hypopigmented variant of cutaneous T-cell lymphoma |
- More common in patients with skin of colour
- Common bathing trunk distribution with associated skin atrophy and eczematous changes
- Diagnosed by clinicopathological correlation and thus requires skin biopsy
|
| AA differential diagnosis not to be missed: Biopsy should not be considered in all patients with hypopigmentation. Patients with pigmentary issues should be considered for referral to a dermatologist to ensure differential diagnoses are not missed, to optimise management and to provide a multidisciplinary approach to care. |
Answer 3
Early intervention changes the natural history of the condition and increases the chances of complete repigmentation.3 Thus, referral to a dermatologist with expertise in vitiligo is recommended alongside sharing resources from trusted sources such as the Global Vitiligo Foundation and the Vitiligo Association of Australia. Referral to a psychologist or psychiatrist should also be considered if screening suggests depression, anxiety or other psychiatric comorbidities.
Therapies available for vitiligo include:
- Topical therapies: Lesions on the face, neck and intertriginous areas and lesions in children should be treated with calcineurin inhibitors such as tacrolimus and pimecrolimus, whereas lesions elsewhere on the body might be treated with potent to ultrapotent corticosteroids in a cyclical fashion.8 There is no evidence that topical calcineurin inhibitors increases the risk of malignancy, despite the black box warning remaining.9 Topical tacrolimus can be considered with prescription from compound pharmacies.
- Phototherapy: Narrowband ultraviolet B light therapy (NB-UVB) is commonly used and is indicated when >5–10% of the body surface area (BSA) is affected, in rapidly progressing vitiligo or when treatment has been refractory to topical therapy alone.8 NB-UVB acts to stimulate differentiation of melanocytes while having a local immunosuppressive effect within the skin. Long-term NB-UVB therapy has not been shown to increase the risk of melanoma or non-melanoma skin cancers in those with vitiligo.10
- Targeted UVB phototherapy: Targeted UVB phototherapy such as excimer laser is used when <10% BSA is affected to repigment small areas of involvement.8 An advantage of this type of therapy is limiting exposure only to vitiligo lesions, thereby minimising side effects in non-vitiligo-affected skin. However, this does not prevent new spots from appearing.
- Immunosuppressive therapies: Oral corticosteroids are typically used when vitiligo is rapidly progressive. Clinical signs of rapidly progressive vitiligo include confetti depigmentation, koebernisation and trichrome vitiligo, and should herald a more urgent referral to a dermatologist. Low-dose betamethasone or dexamethasone prescribed in a weekly pulsed manner for a maximum of two to three months is the most common regimen used.11 Other immunosuppressants, including methotrexate, have been trialled but are not commonly used; they might be considered by dermatologists who specialise in vitiligo, but their use might be limited by side effects.11 Promising new targeted biological therapies are now emerging for the treatment of vitiligo, including Janus tyrosine kinase (JAK) inhibitors such as tofacitinib, ruxolitinib and ritlecitinib.8
Cosmetic camouflage is also available as an adjuvant or alternative therapy in patients with vitiligo. This involves concealing vitiligo lesions with self-tanning products, liquid dyes, pigmentary foundation and via depigmenting unaffected surrounding areas of skin. Its use is associated with a significant increase in quality of life, including raised self-esteem and confidence.12 Cosmetic camouflage is an important option to discuss with patients because repigmentation does not occur immediately with medical therapy and it provides a solution for cosmesis. Microtattooing is not recommended because this can trigger further vitiligo lesions by virtue of koebernisation.
Surgical therapies might be considered in patients with non-responsive, stable vitiligo and are most successful in those with late-stage segmental vitiligo.8 Surgical options include tissue grafts, whereby solid tissue is transferred from donor to recipient, and cellular grafts, which involve the transfer of suspensions of melanocytes to a larger BSA of the recipient.8 Non-cultured epidermal melanocyte cell grafting remains the most efficacious of the surgical therapies available for vitiligo.8
Many cultural and ethnic groups have firmly held beliefs about the causes of and treatments for vitiligo. It is vital that the clinician approaches the patient and their family in a culturally sensitive manner while exploring the beliefs and cultural assumptions that they might harbour about the condition. Each patient might disclose different themes regarding their vitiligo during the consultation, ranging from that of feeling outcast to having a sense of solidarity with the vitiligo community, or even expressing their vitiligo as beauty.13 These topics need to be sensitively and carefully explored to ensure greater understanding of the patient’s perspectives and to optimise both patient–doctor rapport and treatment compliance.
Key points
- Vitiligo is not purely a cosmetic condition, but is a progressive autoimmune disease with potentially severe psychosocial impacts.
- There is no one-size-fits-all approach for vitiligo given that the condition presents differently for each patient. This is reflected in the different management approaches that are used.
- Pulsed steroid therapy is typically used for widespread progressive vitiligo, whereas ultrapotent topical steroids might be used for locally progressive and active vitiligo.
- New and emerging therapies for vitiligo provide promising solutions to an otherwise therapeutically challenging pigmentary disorder.