Case
A male infant, aged 11 weeks, was referred by their general practitioner to the paediatric clinic with concerns of torticollis noted within the first few weeks of life. Pregnancy was complicated with a maternal urinary tract infection from 34 weeks gestation leading to the induction of labour at 38+4 weeks gestation. There were no immediate postnatal complications. The infant had had two previous admissions to hospital with bronchiolitis but recovered well. His immunisations were up to date and he was thriving.
His mother reported that he favoured looking to the left side with his neck turned to that side. He would track his eyes to both the right and left side, but react less to loud noises on the right. At the time of presentation, he had already been referred to a paediatric physiotherapist for the management of congenital torticollis.
On assessment, he kept his head turned to the left in the supine position without a chin tilt to the opposite side and tracked his eyes to visual stimuli. On passive movements, we were able to move his head nearly 90° to the right side without resistance. Interestingly, when placed prone, he actively moved his head from the left to the right side. There was no tightening or masses felt over his sternocleidomastoid on either side. He had no plagiocephaly and he had soft fontanelles, and the rest of his systemic examination was unremarkable.
Question 1
What is congenital torticollis?
Question 2
How do you differentiate between congenital and acquired torticollis?
Answer 1
Congenital torticollis is a clinical diagnosis defined by the finding of a twisted or rotated neck. At this age, congenital torticollis is commonly seen and refers to a postural deformity of the neck due to unilateral shortening or tightness of the sternocleidomastoid. It is usually seen by two to four weeks of age. In contrast, acquired torticollis can be seen at any age.1
Answer 2
Differentiating the causes of torticollis is primarily done by a clinical examination. In congenital torticollis, onset should have been noted at birth or soon afterwards. The head and ear will be seen tilted towards the affected side and the chin to the opposite side. Passive movements of the neck when stabilised in the supine position will be restricted and a characteristic sternocleidomastoid mass might be felt. Ocular, spinal and neurological examinations are important to detect possible non-muscular causes.2
Case continued
Due to the clinical findings, which did not fit with a typical congenital torticollis of muscular origin, a head ultrasound was arranged, which showed a large area of missing parenchyma in continuity with the body of the left lateral ventricle with dilated lateral ventricles. Magnetic resonance imaging of the brain was arranged to further delineate, which showed a large left frontal lobe porencephalic cyst communicating with the left lateral ventricle (Figure 1). There was also evidence of previous intraventricular haemorrhage with associated hydrocephalus and minor mass effect.
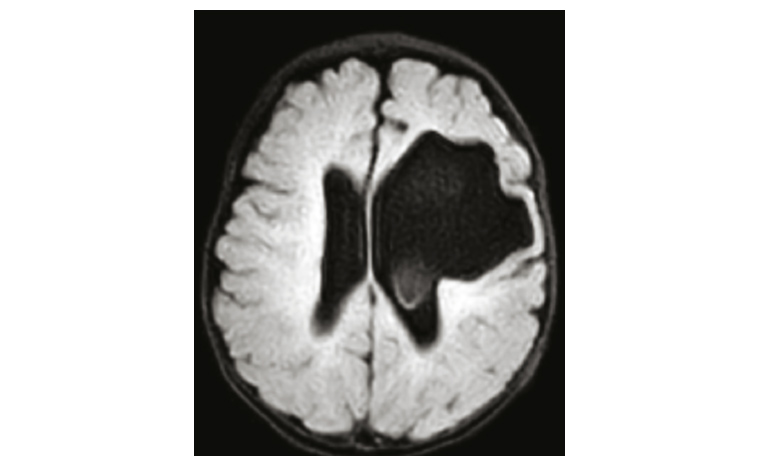
Figure 1. Magnetic resonance imaging of the brain, T2-weighted fast fluid-attenuated inversion recovery, axial view. The image shows a large porencephalic cyst communicating with the left lateral ventricle. Taken from the patient’s record with consent.
Question 3
Why is it important to consider other differential diagnoses?
Question 4
What are the other differential diagnoses to consider?
Question 5
When should a specialist referral be considered?
Answer 3
Congenital torticollis is a common presentation. Although the predominant cause is muscular, there are various examples in the literature of the devastating consequences of misdiagnosing a progressive neurological lesion.3–5 Although we understand it might be impractical to expect primary practitioners evaluating a child in a busy clinic to rule out the numerous neurological causes, we aim to highlight the importance of having a high degree of suspicion during these consults.3–5
Answer 4
Table 1 lists a number of differentials to consider.6
| Table 1. Differential diagnoses of congenital torticollis |
| Postural |
Postural preference with no muscle involvement |
Muscular and
ligamentous causes |
Tightness of sternocleidomastoid, congenital absence of sternocleidomastoid, sternocleidomastoid cyst, syndromic (Trisomy 21, Marfan syndrome), achondroplasia |
| Bone |
Congenital scoliosis, fusion anomalies |
| Central nervous system |
Arnold–Chiari malformation, cerebral palsy, porencephaly |
| Other causes |
Sandifer syndrome (GORD), infectious causes (neck abscesses), vascular/ischaemic events in utero |
| GORD, gastroesophageal reflux disease. |
Answer 5
The following red flags denote clinical concern necessitating a referral:7
- torticollis noted after six months of age
- acute onset of torticollis
- absence of typical tilt, and passive restriction of movement (mentioned above)
- fever and other associated infective symptoms
- abnormal eye movements
- associated developmental delay
- failure to thrive.
Case continued
The patient was diagnosed as a unilateral presentation of cerebral palsy after he scored 56 with seven asymmetries on the right on the Hammersmith Infant Neurological Examination (HINE).7 He is also expected to have motor impairment on the right side of his body due to the extent of the porencephalic cyst involving motor tracks. He will continue to have regular general paediatric follow-up and early intervention therapies.
Key points
- Torticollis in infants has a broad aetiology and although congenital muscular torticollis is the most common, other differentials must be considered.
- Thorough clinical evaluation and neurological assessment is necessary in infants with torticollis.
- Consider early referral to tertiary services in infants with red flags or unusual examination findings.