Medicines are increasingly used to control risk factors; lipid-lowering medicines are recommended for cardiovascular disease (CVD) and risk.1 Since 2016–17, statins have been the most commonly prescribed medicines in Australia2 and, in 2016, they were prescribed to over 40% of older people.1 Many other chronic conditions are commonly comorbid with CVD, including diabetes, chronic lung disease, mental health disorder and autoimmune conditions,3 so patients taking statins are often prescribed multiple additional medicines.
Polypharmacy is described as taking five or more concurrent medicines;4 the polypharmacy rate among US patients with CVD aged ≥65 years increased from 24% in 2000 to 39% in 2014.5 As medicine number and complexity increase, so do the risks of adverse interactions and events,4 and reduced patient adherence.6 In Australia, most longer-term medicines have been dispensed in monthly quantities, also necessitating frequent pharmacy visits, although Pharmaceutical Benefits Scheme (PBS) changes in September 2023 have begun to address this with 60-day supply for some items.
People incur financial cost for medicines. International research shows that this is associated with reduced adherence, adverse outcomes and increased expenditure for the healthcare system.7–9
The Australian PBS mitigates cost with a fixed patient co-payment for each prescription dispensed. In 2019 this was capped at $6.60 for low-income and disadvantaged ‘concessional’ beneficiaries, and at $40.30 for general beneficiaries. The PBS-published Dispensed Price for Maximum Quantity (DPMQ) indicates, for each medicine, the maximum chargeable by pharmacies, including all fees and mark-ups.10 Co-payments from registered family members contribute towards a PBS safety net threshold; in 2019 this was $390 for concessional and $1550.70 for general beneficiaries. After reaching this threshold, co-payments were removed for concessional beneficiaries and reduced to $6.60 for general beneficiaries.11
The aim of this study was to investigate the largely unknown medicine burden and costs for both general and concessional beneficiaries dispensed with lipid-lowering medicines in Australia.
Methods
This was a cross-sectional analysis of the 2019 PBS dataset (a de-identified 10% random sample of all PBS prescriptions) over the calendar year. The dataset included pharmacy location (state), medicine item code, strength, quantity dispensed, date dispensed, number of repeats and concession/safety net status. From this source, a subset was generated of all patients that year dispensed one or more prescriptions for a statin, ezetimibe, fibrate or proprotein convertase subtilisin/kexin type 9 (PCSK9) inhibitor. Demographic data included sex and the dates of birth and death. PBS medicine item codes were matched to full Anatomic Therapeutic Chemical (ATC) codes, identifying unique medicine preparations, and to the DPMQ.12
Patient age was calculated at the date of first dispensing in 2019; those aged under 18 years or who died during the year were removed from the analyses. Analyses were stratified by age group because age was not linearly related to dependent variables examined. People were classed as concessional/general beneficiaries according to their status for >50% of dispensing. For each individual, we determined the total number of prescriptions dispensed and the number of unique medicine preparations. Medicines that were prescribed with two or more repeats or in quantities of ≥100 were defined as longer-term medicines.
For each prescription dispensed, cost to the patient was estimated using the co-payment level corresponding to their PBS status at that time or the DPMQ, whichever was lower. Comorbidity was ascribed for diabetes, hypertension and congestive heart failure by using previously validated algorithms relying on medication ATC classification.13
Non-parametric tests of significance were used throughout and multivariable logistic regression via a backwards stepwise approach, which was performed using the upper quintile of variables. All analyses were performed using Stata software (Stata/IC v14.1; StataCorp, College Station, TX, USA).
This study was approved by the Monash University Human Research Ethics Committee (Project ID 22877). The analysis application was approved, and the final manuscript noted by Services Australia External Request Evaluation Committee (RMS 1112).
Results
Demographics
The cohort numbered 298,083 individuals; 49% identified as female (the rest male) and nearly 73% were aged >60 years. Approximately 62% of patients were concessional beneficiaries for >50% dispensing. By the end of the year, 0.8% of general beneficiaries and 22.7% of concessional beneficiaries were recorded as having reached their respective safety nets.
More than 12 million prescriptions for any medicine were dispensed. The majority (89.9%) of lipid-lowering prescriptions were for statins alone, and 97.8% of patients were supplied with at least one prescription containing a statin. Around one-quarter (26.6%) of the cohort was identified as having diabetes and nearly two-thirds (63.3%) with hypertension. Congestive heart failure was identified in 4.9% of the cohort (Table 1). General beneficiaries had a greater prevalence of comorbidity than did general beneficiaries (Appendix 1, available online only).
| Table 1. 2019 Pharmaceutical Benefits Scheme 10% sample: Demographic characteristics of patients supplied lipid-lowering medication (n=298,083) |
| |
n |
% |
| Age group (years) at first prescription supply in 2019A |
|
|
| 18–30 |
1022 |
0.34 |
| 31–45 |
12,148 |
4.08 |
| 46–60 |
68,453 |
22.97 |
| 61–80 |
173,939 |
58.36 |
| 81–99 |
42,467 |
14.25 |
| Sex |
|
|
| Male |
158,396 |
53.14 |
| Female |
139,687 |
48.86 |
| Concessional status |
|
|
| General ordinary+safety net |
113,924 |
38.22 |
| Concession ordinary+safety net+other free |
184,159 |
61.78 |
| Lipid-lowering therapy type |
|
|
| Statin monotherapy |
267,956 |
89.89 |
| Ezetimibe monotherapy |
6420 |
2.15 |
| Statin–ezetimibe fixed-dose combination |
16,292 |
5.47 |
| Statin plus ezetimibe (separate) |
7253 |
2.43 |
| PCSK9 inhibitor±another lipid-lowering medicine |
162 |
0.05 |
| Comorbidities |
|
|
| Diabetes |
79,391 |
26.63 |
| Hypertension |
188,576 |
63.26 |
| Congestive heart failure |
14,670 |
4.92 |
| AUnspecified n=54. PCSK9, proprotein convertase subtilisin/kexin type 9. |
Prescriptions dispensed
The total annual number of prescriptions dispensed increased significantly with age. The median was 19 (interquartile range [IQR] 9–35) for those aged 31–45 years, rising to 37 (IQR 23–57) and 53 (IQR 36–74) for those aged 61–80 and 81–99 years, respectively (Table 2). One-quarter of the cohort had ≥57 prescriptions dispensed, with age 80–99 years independently associated with a fourfold increase in the odds of reaching this level, compared with age 18–30 years (Table 3).
| Table 2. Number of prescriptions dispensed, number of unique medicines, number of longer-term medicines and estimated cost to patients on lipid-lowering therapy in 2019 |
| Patient category |
Total number |
Cost to patients ($) |
| Prescriptions dispensed |
Unique medicinesA |
Unique longer-term medicinesB |
| Whole cohort (n=298,083) |
36 (21–57) |
7 (4–10) |
4 (3–7) |
286 (176–436) |
| Age group (years)C |
|
|
|
|
| 18–30 (n=1022) |
15 (7–29) |
5 (3–8) |
3 (2–5) |
169 (86–328) |
| 31–45 (n=12,148) |
19 (9–35) |
5 (3–8) |
3 (2–5) |
247 (126–437) |
| 46–60 (n=68,453) |
25 (14–42) |
5 (3–8) |
3 (2–5) |
338 (182–562) |
| 61–80 (n=173,939) |
37 (23–57) |
7 (4–10) |
5 (3–7) |
273 (176–416) |
| 81–99 (n=42,467) |
53 (36–74) |
9 (6–13) |
6 (4–9) |
286 (201–297) |
| Patient sexC |
|
|
|
|
| Male (n=158,687) |
34 (20–55) |
6 (4–9) |
4 (3–7) |
293 (82–459) |
| Female (n=139,687) |
37 (22–59) |
7 (5–11) |
5 (3–7) |
280 (176–416) |
| PBS statusC,D |
|
|
|
|
| General (n=113,924) |
24 (13–38) |
5 (3–7) |
3 (2–5) |
438 (234–760) |
| Concessional (n=184,159) |
45 (28–66) |
8 (5–12) |
5 (4–8) |
242 (163–351) |
| Lipid-lowering medicineC |
|
|
|
|
| Statin only (n=267,956) |
35 (20–56) |
7 (4–10) |
4 (3–7) |
280 (176–424) |
| Other medicines (n=30,127) |
41 (25–64) |
8 (5–12) |
5 (4–8) |
345 (215–559) |
| ComorbiditiesC,E |
|
|
|
|
| DiabetesC (n= 79,391) |
51 (33–74) |
9 (6–13) |
6 (4–9) |
364 (241–546) |
| No diabetes (n=218,692) |
31 (18–49) |
6 (4–9) |
4 (2–6) |
260 (163–403) |
| HypertensionC (n=188,576) |
43 (28–63) |
8 (5–11) |
5 (4–8) |
319 (215–468) |
| No hypertension (n=109,507) |
22 (12–40) |
5 (3–8) |
3 (2–5) |
221 (129–377) |
| Congestive heart failureC (n= 14,670) |
74 (53–99) |
14 (10–18) |
9 (7–12) |
378 (273–465) |
| No congestive heart failure (n= 283,413) |
34 (20–54) |
6 (4–10) |
4 (3–6) |
280 (176–431) |
Data are presented as the median (interquartile range).
APrescriptions with different Anatomic Therapeutic Chemical (ATC) codes.
BPrescriptions with different ATC codes and two or more repeats or quantity >100.
CP<0.001 for differences between categories for prescriptions dispensed, unique medicines, longer-term medicines and cost to patients, using the Wilcoxon rank-sum or Kruskal–Wallis tests.
DGeneral: majority of prescriptions were Pharmaceutical Benefits Scheme (PBS) General ordinary or safety net; concession: majority of prescriptions were Concession ordinary or safety net or other free.
EComorbidities identified by the use of a validated tool using drug ATC codes. |
| Table 3. Adjusted odds ratios for the upper quartiles of prescriptions dispensed, unique medicines, longer-term medicines and estimated cost to patients on lipid-lowering medicationA |
| Patient category |
Adjusted odds ratio (95% CI) |
| Prescriptions dispensed ≥57 |
Unique medicines ≥11B |
Unique longer-term medicines ≥7C |
Cost to patients
≥$436 |
| Age group (years; reference 18–30 years) |
|
|
|
| 31–45 |
1.65 (1.28–2.13) |
1.16 (0.94–1.44) |
1.10 (0.89–1.36) |
1.54 (1.26–1.88) |
| 46–60 |
2.23 (1.74–2.86) |
1.23 (1.0 –1.51) |
1.40 (1.14–1.72) |
2.34 (1.93–2.84) |
| 61–80 |
2.67 (2.09–3.42) |
1.33 (1.08–1.63) |
1.68 (1.37–2.07) |
2.69 (2.21–3.26) |
| 81–99 |
4.61 (3.60–5.90) |
2.07 (1.69–2.54) |
2.64 (2.15–3.25) |
3.87 (3.18–4.71) |
| Patient sex (reference male) |
|
|
|
|
| Female |
1.14 (1.11–1.16) |
1.43 (1.40–1.46) |
1.15 (1.13–1.17) |
1.16 (1.14–1.19) |
| PBS status (reference concessional status) |
|
|
|
| General beneficiaryD |
0.28 (0.27–0.28) |
0.32 (0.3–0.33) |
0.33 (0.32–0.33) |
21.94 (21.37–22.54) |
| Lipid-lowering medicine (reference statin) |
|
|
|
| Not statin-only |
1.11 (1.07–1.15) |
1.15 (1.11–1.19) |
1.22 (1.18–1.27) |
1.70 (1.63–1.77) |
| ComorbiditiesE |
|
|
|
|
| Diabetes |
3.23 (3.17–3.30) |
2.66 (2.60–2.71) |
3.48 (3.41–3.55) |
3.04 (2.97–3.11) |
| Hypertension |
2.69 (2.63–2.76) |
2.24 (2.19–2.29) |
3.17 (3.10–3.24) |
2.94 (2.87–3.01) |
| Congestive heart failure |
6.75 (6.48–7.03) |
8.25 (7.92–8.59) |
13.26 (12.64–13.91) |
3.35 (3.20–3.51) |
AAdjusted for age groups, sex, Pharmaceutical Benefits Scheme (PBS) status, non-statin lipid-lowering drug, comorbidities.
BPrescriptions with different Anatomic Therapeutic Chemical (ATC) codes.
CPrescriptions with different ATC codes and two or more repeats or quantity >100.
DMajority of prescriptions were PBS general or general safety net.
EComorbidities identified by the use of a validated tool using drug ATC codes.23 |
The top quartile of total dispensing was strongly associated with comorbid hypertension (odds ratio [OR] 2.69; 95% confidence interval [CI]: 2.63–2.76) and diabetes (OR 3.32; 95% CI: 3.17–3.30) and markedly associated with congestive heart failure (OR 6.75; 95% CI: 6.48–7.03).
Across all ages, total dispensing rates were higher for concessional than for general beneficiaries (Figure 1), who had only one-third the odds of being dispensed ≥57 prescriptions (OR 0.28; 95% CI: 0.27–0.28; Table 3).
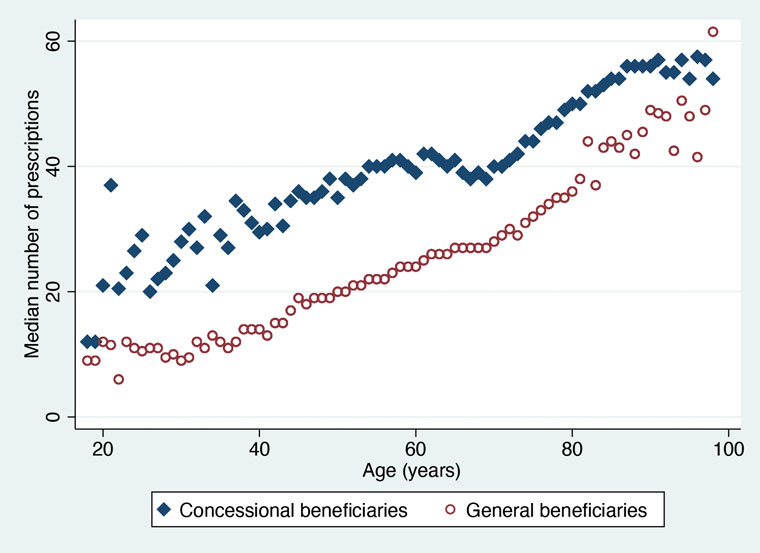 Figure 1. Median number of prescriptions dispensed per person, by age and Pharmaceutical Benefits Scheme status, 1 January – 31 December 2019.
Figure 1. Median number of prescriptions dispensed per person, by age and Pharmaceutical Benefits Scheme status, 1 January – 31 December 2019.
The annual number of unique medicines and unique longer-term medicines dispensed increased with older age. Those aged ≤60 years were dispensed a median of 5 (IQR 3–8) unique medicines and 3 (IQR 2–5) longer-term medicines. For those aged 61–80 years, this increased to a median of 7 (IQR 4–10) unique medicines and 5 (IQR 3–7) longer-term medicines. One-quarter of those aged 80–99 years were dispensed ≥13 unique medicines and nine or more longer-term medicines (Table 2); this age group had double the adjusted odds of reaching the upper quartiles for dispensing (Table 3).
Comorbidity was also associated with increased dispensing of unique medicines and unique longer-term medicines. The adjusted odds of reaching the upper quartile of ≥11 unique medicines more than doubled with diabetes (OR 2.66; 95% CI: 2.60–2.71) and hypertension (OR 2.24; 95% CI: 2.19–2.29) and increased more than eightfold with congestive heart failure (OR 8.25; 95% CI: 7.92–8.59; Table 3). The pattern was similar for reaching the upper quartile of seven or more longer-term medicines; the odds more than tripled with hypertension (OR 3.17; 95% CI: 3.10–3.24) and diabetes (OR 3.48; 95% CI: 3.41–3.55) and increased 13-fold with congestive heart failure (OR 13.26; 95% CI: 12.64–13.91; Table 3).
Cost to patients
The median estimated cost to patients was highest in the group aged 46–60 years, of which 72% were general beneficiaries. Cost was seen to rise steadily for general beneficiaries from about the age of 40 years, whereas concessional beneficiaries had only a minimal increase after the age of 80 years (Figure 2; Appendix 2, available online only). In the cohort overall, older age was independently associated with higher cost; the odds of reaching the upper quartile of cost ≥$436 more than tripled for those aged over 80 years (OR 3.87; 95% CI: 3.18–4.17).
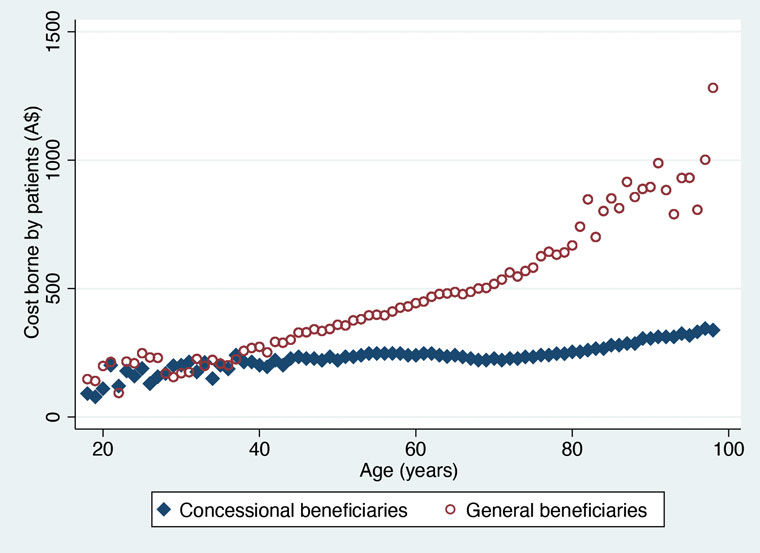 Figure 2. Median Pharmaceutical Benefits Scheme (PBS) pharmaceutical cost borne by patients by age and PBS status from 1 January to 31 December 2019.
Figure 2. Median Pharmaceutical Benefits Scheme (PBS) pharmaceutical cost borne by patients by age and PBS status from 1 January to 31 December 2019.
Compared with concessional patients, general beneficiaries bore significantly higher and wider-ranging costs, with one-quarter estimated to pay $760 or more per annum (Table 2) and only 0.8% recorded as reaching the PBS safety net. General beneficiary status was independently associated with markedly increased odds of paying $436 or more (OR 21.94; 95% CI: 21.37–22.54). This was unsurprising given that concessional beneficiaries had a safety net threshold of $390. However, 17% of concessional beneficiaries and 3% of general beneficiaries reached respective safety net thresholds without a change in PBS status having been recorded (Appendix 3, available online only). This was unexpected given that expenditure by registered family members, not captured by us, could also contribute to the tally.
Comorbidities were also independently associated with cost to patients; the odds of paying $436 or more tripled with comorbid hypertension (OR 2.94; CI: 2.87–3.01), diabetes (OR 3.04; 95% CI: 2.97–3.11) and congestive heart failure (OR 3.35; 95% CI: 3.20–3.51).
Discussion
This was a large cohort of both PBS general and concessional beneficiaries using lipid-lowering medicines. We found that individuals commonly experienced high-frequency dispensing of multiple additional medicines, associated with older age, comorbidity and PBS concessional status. General beneficiaries frequently incurred significant cost, and patient expenditure may not always have been captured and registered for the PBS safety net.
Our results are consistent with previous Australian data showing that 20% of people aged ≥65 years were taking five or more concomitant medications;14 another study found a polypharmacy rate of 28% for people aged ≥70 years.15 Our cohort was selective for CVD risk, so it is unsurprising that dispensing rates were higher for longer-term medicines. Our results are also consistent with US data in the older population with CVD, of whom 39% experienced polypharmacy.5 Medicines are initiated by various medical specialists and hospital staff, as well as by general practitioners, often following best practice guidelines for the management of particular conditions. However, general practitioners are likely aware of their patients’ overall health, values and circumstances, and so are well placed to raise the issue of medicine burden. A periodic medicine review may identify medicines no longer indicated, while regimes may be simplified with the appropriate use of combination and long-acting preparations.16 Collaboration with a pharmacist can be helpful in keeping abreast of the changing options and availability of products; for example, via a domiciliary medication management review. General practice involvement in research can contribute to good-quality outcome data for various population groups, necessary to guide appropriate prescribing.
The high-frequency prescription dispensing that we found will be somewhat ameliorated by recent changes to the PBS allowing 60-day supply of some medicines. This strategy could be extended for stable medicines, analogous to the longstanding four-month supply for oral contraceptives. It is difficult to keep dispensing synchronised when medicines are supplied in both 28- and 30-day packs.
The estimated medicine cost for general beneficiaries was consistent with previous Australian findings that it takes up a substantial proportion of low-income household expenditure, imposing a financial strain.17,18 This may adversely impact medicine adherence,18-22 risking poorer health outcomes and increased costs to the healthcare system.7,8,23 Previous PBS co-payment changes were found to impact dispensing and presumably medication compliance.24 The costs we estimated will be somewhat ameliorated by a recent PBS co-payment reduction combined with increased dispensed quantities.
Only a small percentage of general beneficiaries were recorded as reaching the PBS safety net. Those on a low income and with chronic illness have previously been found to experience financial stress for many months while waiting to reach the threshold.17 Adherence to statin therapy was shown to improve when the safety net was reached.25 The recent PBS changes have lowered the threshold, but for concessional beneficiaries only. General practice staff could assist by ensuring patients are aware of optional family registration and the need for all applicable expenditure to be recorded at both community and hospital pharmacies.
Further insight would be gained with a prospective cohort study collecting data from both prescribers and pharmacies. This could provide information on non-PBS medicines and medicine concurrency, as well as directly recording patient expenditure at the pharmacy level. It could investigate prescription non-filling, perhaps due to cost barriers among general beneficiaries.22,26 Further studies could describe the medicine burden associated with a wider range of comorbidities. It would be useful to investigate PBS safety net functioning with a qualitative study approach.
The strength of the present study was the cohort size and the inclusion of data for both concessional and general beneficiaries. We were limited by a lack of data for medicines dispensed privately or over the counter, including clinician-advised medicines. We did not determine the concurrency of longer-term medicines to inform true polypharmacy rates. ATC codes identified unique medicine preparations, not individual drug constituents of combination products. We may have overestimated costs because we did not allow for the permitted $1 discounting by pharmacies. Recent PBS changes will have somewhat reduced dispensing frequency and out-of-pocket costs, although patterns of association likely remain valid.
Conclusion
People taking lipid-lowering therapy are commonly prescribed multiple medicines for comorbidities, entailing associated frequent dispensing. Non-concessional patients may incur significant out-of-pocket costs. General practitioners are well placed to minimise this medicine burden with periodic medicine review and judicious prescribing. This cohort would also benefit from better understanding of PBS safety-net arrangements.