Melanomas diagnosed by clinicians during skin examinations are more likely to be thinner (T stage 1A/B) than melanomas self-detected by patients.1 As the COVID-19 pandemic has reduced face-to-face medical consultations, reduced diagnoses of thin melanomas and delayed presentations of thick melanomas were anticipated. Consistent with this, the Victorian Cancer Registry recorded a 31% decrease in melanoma notifications between 30 March and 30 June 2020 when compared with 1 February to 27 March 2020,2 although the impact of seasonal variation on these figures is unclear. These authors therefore assessed the impact of COVID-19 on referrals to the Victorian Melanoma Service (VMS), a large, tertiary hospital–based service in Melbourne, Australia.
Methods
This study was performed with approval from the Alfred Health Human Ethics Committee (534/20, 160/20). Retrospective data on new melanoma diagnoses referred to the VMS between 2017 and 2020 were collected from the VMS database. The period of Victoria’s lockdown commenced at midnight on 29 March 2020; as such, referrals for each month pre- and post-lockdown were compared with the same period in previous years. In addition, to determine the effect of COVID-19 on deferment of routine surveillance following a diagnosis of melanoma, 90 patients diagnosed between October 2018 and June 2019 were surveyed by phone over the lockdown period. Data collected during these phone calls related to diagnosis, follow-up, patient timeline (from symptom/lesion onset to biopsy to treatment), any delays of at least one month and the impact COVID-19 had on these elements. Data were analysed using descriptive statistics.
Results
The phone survey identified 21 (23%) patients who reported deferment of their routine surveillance (skin examination or imaging) for at least one month (Figure 1A) because of patient and doctor concerns about contracting COVID-19.
During lockdown, monthly referral numbers for new diagnoses of primary melanoma decreased by 48.0% when compared with the same periods of the 2017–19 triennium (Figure 1B). Reductions were specific to patients referred with melanoma in-situ (MIS) and thin melanomas (7.5 and 7.3 cases per month in April–August 2020, compared with 18.3 and 15.7 in 2017–19, respectively, P <0.0001; Figure 1C), despite normal referral patterns in the months prior to lockdown. The average Breslow thickness of invasive melanomas referred during lockdown was increased (2.70 mm during lockdown, compared with 2.06 mm prior to lockdown, P = 0.03; Figure 1D).
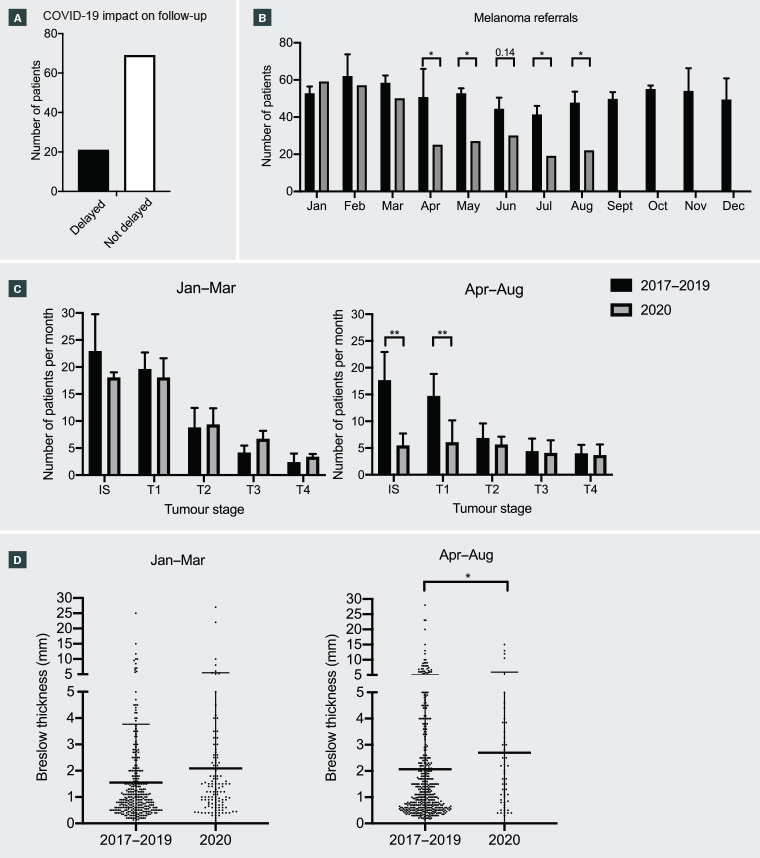
Figure 1. Melanoma referrals at the Victorian Melanoma Service
A. Patients reporting delay in melanoma surveillance (scans of skin examination) as a result of COVID-19, 21 of 90 surveyed; B. New melanoma referrals to the Victorian Melanoma Service per month for 2017–19 compared to 2020; C. Melanoma referrals grouped by tumour stage measured per month for January–March (pre-lockdown) and April–August (during lockdown) for 2017–19 triennium in comparison to 2020; D. Breslow thickness for invasive melanoma referred in January–March (pre-lockdown) and April–August (during lockdown) for 2017–19 triennium in comparison to 2020. Significance was determined using non-parametric t-test and ANOVA.
*P value <0.05
**P value <0.0001
IS, in-situ
Discussion
During Melbourne’s first COVID-19 wave (April–August 2020), referrals to the VMS were substantially reduced. The reductions specifically pertained to MIS and thin melanomas, which are more likely than thick melanomas to be detected by doctors rather than patients.1 This suggests that fewer thin melanomas were detected, likely due to decreased skin checks during face-to-face appointments, which have reduced in the COVID-19 era. This reduction is likely a result of both patient behaviour patterns (decreased attendance) and practice policies (telehealth). Additionally, the reduction might reflect changes in VMS referral patterns during lockdown. As MIS and thin invasive melanomas can often be managed in a primary care setting, this may reflect patient and clinician preference to avoid tertiary centres during the lockdown. One limitation of this study is the inability to identify the cause of this reduction; hypotheses arise on the basis of observations in the data and what has been reported in the registry. Further research involving multiple primary and tertiary centres in Victoria and other areas of Australia would give insight into this.
Although it is difficult to quantify the impact of delayed diagnosis on patient outcomes,3 it is notable that MIS and thin melanoma have excellent prognoses with surgery alone (98–99% five-year survival).4 Delayed presentations of melanoma result in disease upstaging, reduced surgical cures and increased requirements for sentinel lymph node biopsy for staging of thicker melanomas. There was an increase in median Breslow thickness in the study period when compared with previous years. One likely possibility is that this is the effect of a reduction in the number of thin melanomas being referred. Again, this could be because of a reduced number of melanomas being detected, or simply a change in the way thin melanomas are being managed during the study period (in primary care settings, rather than tertiary referral centres).
Referrals of suspicious lesions can be managed safely, even when COVID-19 case numbers are high, via telehealth consultations to identify and triage cases requiring direct examination. In addition, suspected melanoma should be categorised as an urgent review, and the Australasian College of Dermatology recommends these cases be seen with a face-to-face assessment if it is safe to do so.5 To facilitate this, support information is available regarding performing self-skin examinations and taking clinical photos to aid telehealth consultations.6
First published online 22 January 2021.