Case
A nursing home resident aged 80 years presented for an influenza vaccination when he was noted to have a large fungating lesion with rolled edges on his right chest (Figure 1). The lesion was believed to have been present for many months. There was no history of preceding trauma or insect bite, recent travel or immunosuppression. His past medical history was significant for moderate dementia, hypertension, hypercholesterolaemia, benign prostatic hypertrophy, osteoarthritis and alcoholic liver cirrhosis. His medications included dutasteride/tamsulosin, escitalopram, frusemide, perindopril, propranolol and thiamine. He was a retired bricklayer of Scottish heritage with an eight pack-year smoking history.
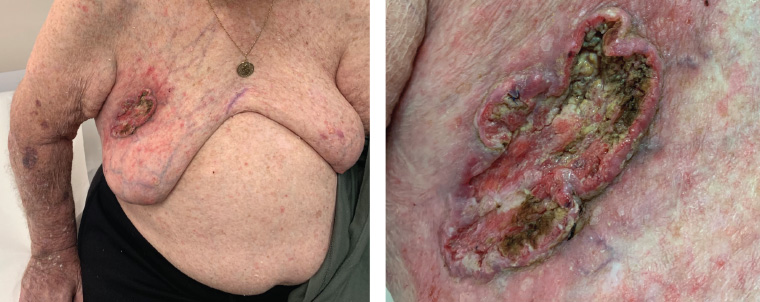
Figure 1. A 10 cm fungating lesion with rolled edges on the right side of the chest
Question 1
What is the differential diagnosis?
Question 2
What initial investigations are required?
Answer 1
A skin cancer would be the primary differential diagnosis, namely a basal cell carcinoma, squamous cell carcinoma (SCC) or amelanotic melanoma. A secondary metastasis from an internal malignancy is possible. An infective aetiology cannot be excluded, such as atypical mycobacterium (eg Mycobacterium ulcerans or M. marinum), cutaneous melioidosis, ecthyma gangrenosum or deep fungal infection. This lesion may also represent an inflammatory dermatosis such as pyoderma gangrenosum or, less likely, a traumatic or pressure ulcer, calciphylaxis, cholesterol embolism, small- or medium-vessel vasculitis, vasculopathy or medication reaction. A venous, arterial or neuropathic ulcer is unlikely given the location of the lesion and absence of diabetes mellitus in the patient’s medical history.
Answer 2
An adequate biopsy specimen needs to be sent in formalin for histopathology. Options include an incisional or large 6–8 mm punch biopsy from the ulcer edge. If considering deep fungal infection or mycobacteria, a ‘fresh’ tissue specimen must be collected and placed on a saline-soaked gauze swab in a sterile container. This tissue can be obtained from a small punch biopsy from the ulcer edge. Fresh tissue must not be placed in formalin and requires prompt collection as the specimen is unpreserved. Swabs should be sent for bacterial and fungal microscopy and culture, which may identify resistant organisms and direct systemic therapy for infected wounds.1 For optimal clinicopathological correlation, it is important that the pathology request form contains relevant medical history; the lesion’s clinical appearance, size and location; and a differential diagnosis list.2
Case continued
Histopathological examination from an incisional biopsy showed an ulcerated, moderately differentiated SCC invading into the subcutaneous fat with no perineural or lymphovascular invasion. Tissue culture and stains were negative for atypical infection. The SCC was classified as high risk for metastasis given the depth of its invasion to subcutaneous fat and diameter of >2 cm. A staging computed tomography scan showed no nodal metastases. The patient was referred to a plastic surgeon and underwent wide local excision with primary closure.
Question 3
What factors increase the risk of developing cutaneous SCC?
Question 4
What factors lead to advanced, neglected skin cancers in the elderly population?
Answer 3
Factors that increase the risk of developing cutaneous SCC include past history of skin cancers, male sex, advancing age, pale skin types, history of extensive exposure to ultraviolet radiation, immunosuppression and presence of actinic keratosis. Less common factors include smoking; ionising radiation; exposure to arsenic, soot and mineral oils; photosensitive genetic disorders; human papillomavirus infection and chronic non-healing wounds.3
Answer 4
Advanced skin cancers are frequently seen in the elderly population. Denial is the most frequent reason for delay in the presentation for diagnosis and treatment of non-melanoma skin cancers, accounting for 70% of cases.4 Reasons for denial include factors relating to patients’ psychological unwillingness to accept the severity of their condition and the need for care (ie thinking that the lesion is insignificant, will go away or can be self-treated; being too busy or fearing the diagnosis).4 In other cases, denial may be indicative of a lack of recognition or understanding of the issue.4 Other factors that can lead to a delay in patients’ seeking medical advice include male sex, living alone, social and geographical isolation, multiple medical comorbidities, low socioeconomic status, inadequate hygiene, incorrect initial diagnosis and fear of treatment.5–7 Self-neglecting behaviours associated with dementia, alcoholism, depression, other mental illnesses, physical impairments and health illiteracy may also underlie advanced presentation of skin cancers in older adults.8,9 Knowledge of these risk factors may enable more prompt diagnosis and treatment of patients before more significant morbidity occurs. As such, it is important that general practitioners are familiar with the risk factors for, and consequences and management of, advanced skin cancers in geriatric patients.
Key points
- Skin cancer should be the primary differential diagnosis in an elderly Caucasian male with a large fungating ulcer.
- An adequate tissue specimen (ie an incisional or large-diameter punch biopsy from the ulcer edge) is important to enable an accurate diagnosis.
- If considering deep fungal infection or mycobacteria, a ‘fresh’ tissue specimen must be collected. Fresh tissue must not be placed in formalin.
- Advanced, neglected skin cancers are frequently seen in the elderly population.
- Multiple factors can lead to a delay in patients’ seeking medical advice, with denial being the most common patient-specific factor.
- Self-neglecting behaviours associated with dementia, alcoholism, mental illness and health illiteracy may underlie advanced presentation of skin cancers in older adults.
- The ceiling of care discussion with elderly patients and their families needs to carefully consider skin cancers such as this, which can lead to significant morbidity and untimely death. If detected early, most skin cancers are successfully treated.