Case
A man aged 72 years requires a walking frame for mobility because of weakness of both legs secondary to poliomyelitis. He presents to the rehabilitation medicine outpatient clinic with soreness and weakness of both hands, which he developed following the use of the walking frame. He also complains of loss of grip strength and tingling of his hands. He is using the heel of the hand to manipulate objects. Examination reveals skin pigmentation and callosities on the ulnar side of both palms, distal to the wrist crease (Figure 1). His general practitioner suspects he has been pressing hard on the frame with the hypothenar area while keeping his wrist ulnar deviated (Figure 2). There is atrophy of the hypothenar, thenar and interosseous muscles of the right hand and thenar muscles on the left hand. Sensation is reduced in the median nerve distribution of both hands and in the ulnar distribution of the right. The Tinel’s sign and phalen’s test are negative. The patient does not have diabetes or any other causes of neuropathy.
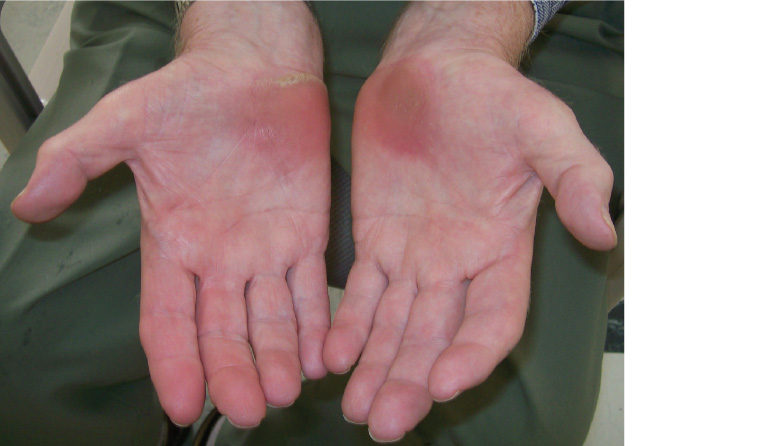
Figure 1. Pigmentation, callosity and atrophy on the ulnar side (hypothenar area) around the Guyon’s tunnel of the right hand and around the carpal tunnel on the left hand from excessive pressure during the use of the walking frame
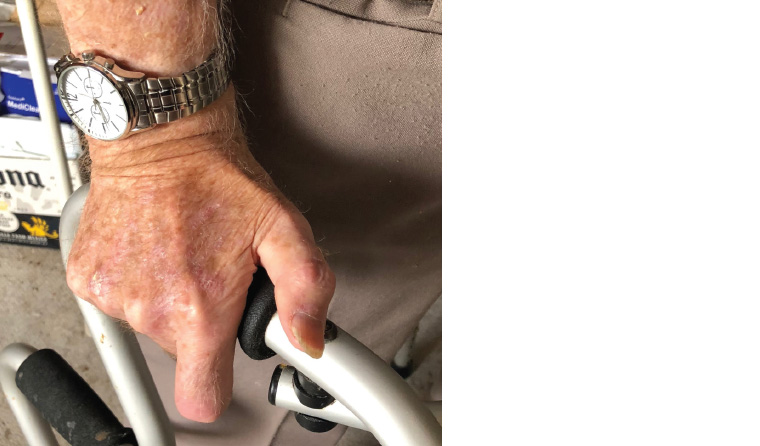
Figure 2. Patient walking with the walking frame. Wasting of the first web space caused by denervation of the first dorsal interosseus and adductor pollicis muscle: a telltale sign of ulnar neuropathy
Question 1
What is the diagnosis?
Question 2
What are the causes of this condition?
Question 3
Which tests are required to establish the diagnosis?
Answer 1
The diagnosis is compression neuropathy of the right ulnar nerve and bilateral carpal tunnel syndrome at the wrist. Pigmentation, callosity and atrophy on the ulnar side (hypothenar) of the right hand are indicative of ulnar nerve compression around the Guyon’s tunnel. This is either caused or exacerbated by the excessive pressure around the wrist during walking with the frame. Wasting of the first web space caused by denervation of the first dorsal interosseous and adductor pollicis muscles is a telltale sign of ulnar neuropathy. On the left hand, the pressure areas are around the carpal tunnel, causing median nerve compression.
Answer 2
Ulnar neuropathies around the wrist have been observed in tool workers, among bicycle riders and after repeated trauma.1 Isolated ulnar nerve palsy has been reported with the use of a walking frame and due to crutch walking.2,3 In this case, simultaneous median and ulnar nerve entrapments resulted from the use of a walking frame by a patient with post-polio paralysis of the lower limbs.
Patients who rely heavily on their hands, without the use of their legs to bear weight adequately while walking with frames, are prone to develop compression neuropathies around the wrists. The walking frame is one of the most common mobility aids, used by many people with impairments of lower limbs for off-loading. Both median and ulnar nerve palsies can occur secondary to pressure around the wrist and can cause significant functional limitations. In late cases where the hand muscles have already undergone atrophy, the motor recovery of those muscles, even after surgical decompression, may be incomplete. For early diagnosis of compression neuropathies, it is important to routinely look at the hands of patients who are taking increased weight through their hands because of a lower extremity problem and using mobility aids. If not picked up early, compression neuropathies can compound the disability.
Answer 3
To establish a diagnosis, the patient requires an ultrasound study looking at the nerve cross-section around the compression, and electrophysiological studies investigating nerve latency, conduction velocity and features of denervation in the innervated muscles.
Case continued
The electrophysiological studies show delayed median motor nerve latencies across the wrists: 14.8 ms and 14.9 ms (right and left wrists respectively; normal: <4.7 ms) and 9.5 ms in the left ulnar nerve (normal: <3.7 ms). There is reduced conduction velocity of 34 m/s bilaterally in the median and 35 m/s in the right ulnar nerve, with small compound muscle action potentials in ulnar innervated muscles and absent sensory action potentials. Ultrasonographical examination reveals an increased cross-section area of 0.2 cm2 and 0.184 cm2 of the right and left median nerves in the carpal tunnel, respectively. The right ulnar nerve is prominent and hypoechoic and measures 0.1061 cm2 in the Guyon’s tunnel. The findings are consistent with severe bilateral carpal tunnel syndrome and a right ulnar nerve lesion at the wrist.
Question 4
What are the treatment options available for this condition?
Question 5
What are the complications?
Answer 4
The treatment options for compressive neuropathies are rest, use of splints, injection of local steroids and surgical release. Mechanical interface and weight-bearing are important considerations in the redesigning of forearm crutches.4 Similarly, an ergonomically designed walking frame should be seen as an important solution that warrants further consideration.
Answer 5
The patient reported progressive loss of grip strength, with difficulties in using cutlery, opening a can and ability to sign. The predominant downside of surgical intervention (eg decompression) is the period of non–weight bearing through the operated hand after surgery. Patients may not be able to manage at home alone if they lose mobility and may decline surgical intervention for this reason. This perpetuates the vicious cycle, as patients continue to use their hands with worsening of the neuropathy. Patients opting for surgery may need an appropriate supported environment while their mobility is severely curtailed as they will be unable to use their hands during the post-surgical healing phase. There are few institutional set-ups (preferably with rehabilitation inputs to prevent decompensation) that can cater for the appropriate extended care needs. Surgery is not a preventive solution, and the long-term outcomes are unknown if patients continue to weight-bear through the walker.
Case continued
The patient is referred for surgical decompression; however, he declines, as it involves a period of non–weight bearing, limiting his ability to live alone. To allow him to take support from his forearms, a gutter frame is prescribed. However, this does not solve the problem, and his hand function continues to worsen.
Key points
- Combined ulnar and median nerve palsy around the wrist can occur when patients with lower limb impairment take considerable pressure through the hands during walking with a walking frame.
- Early diagnosis followed by surgical decompression should be considered to prevent the loss of hand function.
- Following surgery, patients who previously required a walking frame for mobility will need institutional care as they cannot use their hands during the non–weight bearing period.