When disaster strikes, general practitioners (GPs) must rapidly decide how to respond to the healthcare needs of their patients and communities, while often experiencing disaster personally as community members. Research shows that a major burden of disaster healthcare clearly falls within the usual mandate of general practice roles and functions.1–3 This includes addressing acute psychosocial distress, acute lower acuity physical injuries, ongoing management of chronic conditions and coordination of referrals.4–6 However, there is a paucity of research documenting GPs’ frontline contributions to healthcare during disaster responses7 and little guidance for GPs currently facing disasters in their communities on how to best contribute.8
At a policy level, a paucity of understanding of GP capabilities and contributions in disaster response translates into little integration into disaster healthcare planning and response.7–10 At a practitioner level, a lack of inclusion in guidelines and frameworks risks under-preparedness, lack of clarity about responsibilities and isolation in response.8,11 Combined, these represent a significant lost opportunity to reduce disaster health risks and optimise healthcare at a time of overwhelming medical need and demand,10 as well as to provide structured support to local GPs who are exposed personally and professionally.
The aim of this study was to examine and document the roles and experiences of GPs in recent disasters with the goal of providing evidence to help clarify roles and responsibilities of GPs in disaster healthcare.
Methods
Study design
The researchers conducted a qualitative study using semi-structured interviews with disaster-experienced GPs to explore their range of experiences, roles and challenges faced when responding to disasters. The underlying epistemology for the research was constructivist, using an interpretivist theoretical perspective to understand and explain the perspectives of the GPs. A qualitative methodology informed by grounded theory was used to guide the research, supported by NVivo software for coding and thematic development.12–14
Participants
Members or Fellows of any of the GP colleges of Australia or New Zealand (NZ) who had experienced a disaster in a professional capacity in Australia or NZ within the past eight years (2009–16) were invited to the study. For the purposes of this study, disasters were defined as ‘a sudden, calamitous event that seriously disrupts the functioning of a community or society and causes human, material, and economic or environmental losses that exceed the community’s or society’s ability to cope using its own resources’.15
Professional networks were used for purposive snowball sampling. GPs who worked in communities affected by major disasters were identified through GP colleagues, general practice colleges in Australia and NZ, and disaster management professionals. GPs were approached by email or telephone. Further purposive sampling recruited GPs with varying roles and levels of involvement across a range of disasters and geographical locations. The sampling resulted in all recruited participants being from eastern Australia or NZ.
Thirty-eight participants were interviewed before data saturation was reached. This number was necessary to obtain a deep understanding of the broad range of experiences of the participants across different disaster types, roles undertaken, practice and local community characteristics and effects, personal attributes and impact, and levels of involvement.
Data collection and analysis
Data collection using private semi-structured interviews was chosen as it was felt to provide greater confidentiality and comfort for the interviewees. All participants were recruited and all interviews were conducted by the primary researcher (PB). The majority were undertaken at the GP’s practice premises, with any follow-up interviews conducted by telephone. A few interviews were interrupted by the GP’s schedule and were completed at a later date.
Open-ended exploratory questions were developed with reference to the literature and from the experience of the research team to allow a deep exploration of the subject, as there was little previous research available. Refer to Appendix A for the semi-structured question pro forma.
Interview data were audio-recorded and transcribed verbatim. Transcripts were read by two researchers (PB and BR). Ten interviews were initially coded by both researchers together to develop codes and confirm inter-coder consistency. The remaining interviews were divided randomly within disaster type and coded separately. Findings were discussed iteratively with all researchers as they emerged, to revise and confirm the final themes. Sampling continued until thematic saturation was reached.
Reflexivity was enhanced by the different specialty interests and experiences of the research team, highlighting different perspectives from general practice, emergency medicine, psychiatry and disaster management. BR is a psychiatrist with extensive expertise in disaster systems and mixed research; KD is a clinical GP with expertise in healthcare health systems research; WH is a senior medical educator with expertise in community and qualitative research, health policy and program evaluation; PA is an emergency physician involved in disaster management at state and national levels; and PB is a clinical GP with experience in primary care disaster management.
Ethics
Ethical approval was obtained from the Australian National University Human Research Ethics Committee – Protocol 2013/659. Informed consent was obtained from all participants.
Results
Thirty-eight GPs were invited and all agreed to participate. Interviews were undertaken between 2014 and 2016. They were conducted face to face (n = 34) and by telephone (n = 4), with 1–3 interviews per participant. The average interview duration was 43 minutes, ranging from 18 minutes to 90 minutes.
The vast majority of participants had >10 years’ practice in their local area (90%). Most were practice principals, worked in larger practices and/or were located in rural areas. Ninety percent gained their primary medical qualification in Australia (Table 1).
| Table 1. Participant characteristics |
| Characteristics |
n |
| Sex |
| Female |
16 |
| Male |
22 |
| Primary medical qualification |
|
| Australian or New Zealand |
35 |
| International (other than New Zealand) |
3 |
| Years in practice locally |
|
| ≥10 years |
35 |
| <10 years |
3 |
| Employment status |
|
| Partner/principal |
24 |
| Contractor/other |
14 |
| Practice location |
|
| Urban |
9 |
| Suburban |
9 |
| Rural |
20 |
| Practice size |
|
| Large (>4) |
22 |
| Medium (2–4) |
15 |
| Solo |
1 |
| Country of practice |
|
| Australia |
29 |
| New Zealand |
9 |
| Total |
38 |
Collectively, participants had experienced 21 unique disasters spanning nine different hazard types including bushfire, flood, major storm, earthquake, pandemic, terrorist, environmental and technological incidents. Participants were interviewed specifically about their experiences of disasters occurring in Australia and NZ in the preceding eight years (ie between 2009 and 2016). The disasters this included were: the 2009 Victorian bushfires, 2010/2011 eastern Australian floods, 2010/2011 Christchurch earthquakes, 2013 Blue Mountains bushfires, 2014 Hazelwood mine fire disaster, 2014 Lindt Cafe Siege and 2016 Melbourne thunderstorm.
Four key themes were identified from the interviews:
- Responding spontaneously to provide healthcare during the disaster
- Adapting existing GP expertise to disaster healthcare
- Facing personal and professional challenges
- Variation in GP integration.
Responding spontaneously to provide healthcare during the disaster
GPs stepped up to a wide range of roles to address perceived healthcare needs when disaster struck their communities. In Australia, this was despite a lack of clearly defined pathways to guide them in their changed roles (Box 1).
| Box 1. Range of roles general practitioners undertook in providing disaster healthcare |
Keeping the general practice doors open: Business and healthcare continuity
- Business and healthcare continuity despite degrees of adversity
- Infrastructure or supply issues – damage/relocation
- Accommodating other disrupted practices and patient populations
- Addressing modified patient presentations and populations
- Responding to changed patient needs
- Adjusting to change in types of presentation, patient numbers, consultation lengths and patient population
- Prioritising immediate healthcare requirements and targeted preventive activities during high-demand periods
- Changing practice processes and systems temporarily
- Increasing and extending medical outreach, telephone calls and home visits
- Practices ‘on the edge’
- Located outside the disaster ‘zone’ yet experiencing the above effects
Offsite healthcare: General practitioner healthcare provision in an alternative environment
- Within the disaster healthcare response system
- Evacuation centres
- Residential care facilities
- Temporary medical clinics on site
- Member of a local response group
- Outside the disaster healthcare response system
- Spontaneously on site at the incident
|
Business and healthcare continuity
‘Keeping the general practice doors open’ emerged as the key priority in the majority of interviews. All participants showed a strong sense of responsibility and desire to assist in continuing patient healthcare in their local communities, often under adverse conditions and with a risk of personal exposure.
We were all told to leave, but we opened our surgery, because there are all these people that need their scripts. We can’t just close down. Where were they meant to be going? (GP01)
People were standing holding each other up and shrieking in the middle of the street. All I could think of was what’s going on at the surgery? I tried to get [there] as soon as I could. (GP02)
GPs in those flooded areas stayed there to look after their communities rather than getting out. (GP03)
Response roles required flexibility.
We had no power, no computers, no telephones, nothing. Things had fallen off the walls, off the desks. You couldn’t walk into the room … and you just thought, where do you start? (GP02)
Several general practice premises were relocated temporarily or permanently. Some repositioned staff into nearby practices, while others transferred only their patients.
Patient needs changed. GPs noted increased presentations for psychological distress, lost medication, minor injuries, acute exacerbations of chronic conditions and infectious disease outbreaks associated with altered living conditions and crowding.
Variations in patient numbers, both surge and lull, were commonly mentioned. Local patient populations changed with the arrival of emergency responders, alongside evacuation or departure of residents.
About 200 families left the area. All of a sudden they weren’t here. (GP04)
GPs consistently reported an initial increase in consultation lengths; for some disasters, this was prolonged.
Every consultation was five or six minutes of ‘How are you going?’ and ‘How are you affected by the fires?’ (GP04)
Five years later, consultations still include something about the [earthquake]. (GP02)
Researchers noted particular contributions and issues for practices ‘on the edge’, located just outside the disaster ‘zone’. These practices were not considered ‘disaster affected’, but they supported patients and practices that were more directly affected. Two GPs, located two hours and half an hour from the incident, respectively, illustrated the impact:
There was a really big immediate impact. Something like 2000 people came through here. It put a lot of pressure on us, and a couple of our GPs did head up to [the disaster site] to assist. Then of course that meant there was nobody here. (GP05)
The first day was shocking. It was pretty horrendous, especially for those who’d actually lost their family member, or members. It was horrific. All the seats were filled. It was hard for us all because we knew these patients too, and who had just died and … We were all upset. Everyone was on alert. (GP06)
A few participants experienced incidents where airborne environmental hazards such as smoke or pollen created a widely dispersed effect on an urban population.
We knew there was a storm, so although given no information on what was happening out in Melbourne, we guessed it was allergies due to the storm. Just before 9.00 pm there was an increasing stream of patients presenting with acute respiratory distress. We did what we normally do. Just managed the surge then back to normal. (GP07)
Another disaster experienced by an outer-Sydney GP as having far-reaching ripple effects involved fear.
The siege wasn’t just in Martin Place, the siege was actually all over the city. (GP08)
Offsite healthcare: General practice healthcare provision in an alternative environment
Much less frequently, GPs were involved in healthcare provision outside the customary medical practice environment. This included working in an evacuation centre, consulting in a tent, setting up a clinic in a church or attending at the incident site solo or as part of a response team.
In a church:
Three days later we were still isolated. I just had my doctor’s bag. It was at that stage I’m sitting there thinking, this is getting a bit serious now. Between the three of us, we started to organise a little mini hospital. (GP09)
Most offsite roles were immediate and lasted hours to several days. Following a catastrophic bushfire, one semi-permanent medical clinic staffed with offsite GPs continued for several years and evolved into the local general practice.
Adapting existing GP expertise to disaster healthcare
The unique characteristics of general practice healthcare emerged clearly from the data driving the healthcare provided by GPs during these disasters. The data showed GPs intuitively applied their usual person-centred, accessible, first-contact, continuous, comprehensive, coordinated healthcare to individuals within a family- and community-focused environment16–22 in the disaster roles they assumed.
This approach, as shown in Figure 1, was maintained but adapted during the disaster to sustain local primary healthcare as practicable.
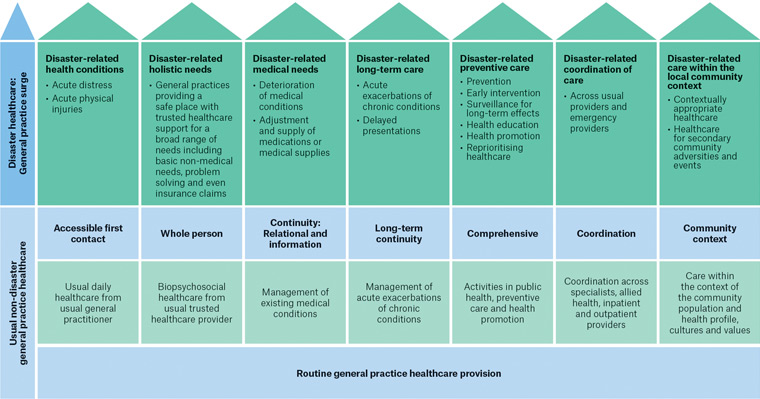
Figure 1. Characteristics of care driving the general practitioner response during disasters, compared with non-disaster times
Click here to enlarge
Continuity
Continuity emerged as the strongest characteristic of healthcare, provided by the majority of participants: the benefits of information continuity for management of chronic conditions, and relational continuity for providing a trusted familiar healthcare source.
And even as a GP, you think, ‘Oh, come on, it’s just a script’, and it’s hard to see the importance of doing that as opposed to being out there pulling people out of broken buildings. But everybody has got their part to play in keeping the normal health functions going. Keeping people’s [chronic obstructive pulmonary disease], heart failure, asthma and diabetes under control so that they can be healthy enough to cope with their own lives is actually really important. And then there’s the mental health thing. That’s just vast. And it started immediately. It really did. (GP10)
Long-term continuity of care
Long-term continuity of care provided an enhanced understanding of the disaster’s impact for proactive surveillance and management:
We are still getting [regular patients] coming in for the first time now, seven years later, for [effects from the disaster] to be addressed. (GP11)
I have noticed that for people who have had trauma early on as children perhaps, a disaster like this retriggers that trauma. (GP01)
The shared experience: In a community context
For the majority of GPs, the disaster was a shared experience with the local community. This afforded a deeper understanding of the healthcare needs and a real-time understanding of the evolving effects on the community.
Many felt the community turned to them as trusted local health professionals.
That was the big thing after the earthquake, is that it didn’t matter where the GP was, [patients] found them … patients would have walked … across the city to get to their own GP. (GP19)
We were here about 7.30 am in the morning and we had patients at the front door. We had two families at the door covered with ash ... they were here for ages ‘cause they were upset. (GP20)
A perceived lack of understanding of local context among other responders was the most frequently mentioned source of frustration.
There was a misreading of what people actually needed and what the people were all like there, and local GPs kept telling anybody who would listen. (GP12)
Personal and professional challenges
Challenges experienced by Australian and NZ GPs showed consistency across different types of disasters. Key emerging issues included:
- being personally affected as a member of the affected community
- the dichotomy between looking after patients while making sure their own family was safe
- the enduring nature of effects from the disaster
- profound fatigue compounded by long, sustained working hours.
The degree of impact on GPs and their practices varied from minimal to profound. Those more affected experienced loss of practice and staff homes; loss of lives of friends, colleagues and patients; loss of community; a damaged local environment and a changed reality.
The majority of GPs articulated a sense of immersion in sharing the adversity with their communities, living closely with family and friends as community members in the changed environment.
What happens to our community affects us personally as well as professionally. One staff member had to suddenly run out when her house started burning. (GP01)
On the day that all those houses burnt down, I remember coming into work. There was this sort of palpable anxiety – patients, staff, everybody was very anxious. My house is only two kilometres from the 200 houses that burnt down. There was a real mix of work responsibility but also being quite frightened for your own family and kids. (GP13)
The whole community wanted to talk about it. I think I became fatigued talking about it. (GP11)
It was traumatic listening to all those stories from patients. In those first few weeks when there was no information, we would see a patient and say oh, and do you know what’s happened to the whatever family? And wait to be told they’re fine, lost their house, or, this person has died, or I haven’t seen them, or I don’t know. (GP11)
Variation in GP integration
NZ GPs felt better integrated and valued within the broader disaster-response system when compared with the Australian GP cohort. NZ participants felt better prepared for the disaster and more integrated into the broader response.
Preparedness for the emergency
None of the Australian GPs felt prepared for the event they experienced. However, most NZ GPs reported a level of general disaster preparedness, despite those from Christchurch clearly articulating they never expected they would experience a major earthquake.
Australian GPs felt other responders’ misconceptions of their capabilities contributed to limited a priori involvement.
People don’t know what we do. They think all we do is write scripts and refer people. (GP14)
Integration into the response
In contrast to the NZ cohort, the majority of Australian GPs were unclear of their role or the broader disaster-response system, and how they might best contribute.
There’s not a sense of an overall plan for a medical response within the community, amongst the GPs, that I have any knowledge of – or how I can contribute. (GP15)
But no one was sitting in the control centre saying, ‘What are we going to do about medical emergencies? Like, are there doctors up there? Are there doctors who are staying up there?’ (GP16)
There were a lot of services available, and it was really hard to know what was going on and who was responsible. (GP14)
Sense of value of their contribution
All NZ participants agreed that GPs added significant value to disaster response and recovery, a period when their local communities’ health was at risk. The majority of NZ GPs felt included in systems of response and valued by other disaster responders.
It’s wonderful to think in terms of bringing in help, but the help is not as good as the folk [GPs] that are actually already on the ground. (GP17)
After the first 12, 18 hours, there was very little hospital work that was needed. They’d done all the acute trauma. There was nothing else coming out. But it was trying to ensure that healthcare remained viable out in the community, which was the big problem. (GP18)
However, there was a general sense among Australian GP interviewees that their contribution was poorly valued and understood by other disaster health professionals.
It’s like we were sort of completely out of [the disaster]. We’re not important, the hospital was important but GPs just didn’t really matter. (GP01)
Whether included in systems of care or not, Australian and NZ participants described a strong sense of professional responsibility and desire to contribute to their patients’ care at this time. For some Australian GPs, this translated into a sense of helplessness in the face of the catastrophe and frustration at not being included in formal responses to help their patients and communities.
Discussion
The novel contribution of this research is to show that GPs in this study – as local, embedded medical professionals – were actively involved in disaster healthcare, both acutely and longer term. On site when disasters occurred, study participants responded with a powerful sense of responsibility for their patients and communities, taking on a rich variety of roles to contribute to disaster healthcare relevant to general practice.1–5 Roles adopted by GPs were strongly driven by the characteristics of routine general practice healthcare adapted to accommodate the adverse situation. GPs defined their own roles as they enacted them. These were focused on patients’ primary healthcare needs, contingent on the limitations of the new situation and on the community context. The results of this study add to the limited research related to GP involvement in disasters and respond to the request for research documenting primary healthcare activities in this field.7
Despite abundant scientific evidence for the crucial need for strong primary healthcare to support a strong healthcare system,1–5,17,19–23 and the documented high burden of primary healthcare needs in disasters,1–5 most of the effort and resources in disaster healthcare still focus on acute secondary and tertiary services.23
If you don’t involve primary health care more broadly and general practice specifically, you’re missing most of the health system. (GP19)
While professional roles were unhesitatingly assumed during these traumatic adversities, effects on personal and professional wellbeing were apparent among the participants. This is consistent with the expansive literature on the impact of disasters on individual and responder wellbeing in general6 and the limited literature on the impact specifically on GPs.11
This study supports the need to clearly outline the capabilities GPs can contribute to disaster healthcare and the need to integrate these contributions with other levels of healthcare to promote a ‘whole of health system’ response situated in the unique context of each affected community.9,24 This is important from the perspective of supporting the healthcare of the community in a disaster but also from the perspective of supporting the health and wellbeing of the GPs themselves.11
In Australia, since the first disaster (2009) in our sample, there has been more national and state attention given to GP disaster responsiveness, although explicit GP involvement in disaster policy remains minimal. Persistent underutilisation of GP contributions risks further compromise to the health of those affected by disaster.3
NZ’s system is shifting the paradigm. Greater certainty of roles, responsibilities and value exists among NZ GPs, as NZ has a greater degree of GP integration into disaster healthcare preparedness and response systems, developed over years of collaboration and involvement in planning.25 Internationally, however, the vast majority of disaster healthcare systems have yet to embrace this shift.
Strengths and limitations
Study strengths include the depth and diversity of experience among the 38 GP participants. The in-depth expertise of the lead researcher (PB) in the primary healthcare disaster medicine field influenced recruitment positively, but it may also have skewed recruitment to known professional networks and data interpretations. However, diverse perspectives within the research team during data analysis allowed researcher triangulation that assisted with trustworthiness of interpretations.
Although a wide sample of locations and disasters over a seven-year period were included, most were within the eastern seaboard of Australia and the NZ earthquakes; transferability to disasters in different contexts may therefore be limited, as it was not a nationally representative sample. Conducting disaster research, including recruitment of participants, has particular challenges, such as the unpredictability of the timing and location of disasters. This makes random representative sampling more challenging.26 Most participants were from Australia; differences found with NZ GP participants may not be evident with a larger NZ sample. Through purposive sampling, this study nevertheless offers an in-depth exploration of a wide range of experiences within the disasters sampled.
Implications for Australian general practice
To optimise healthcare outcomes for communities and patients, and protect the wellbeing of local GPs, the authors suggest that GPs and GP organisations need to consider their roles in disaster response, beginning with pre-disaster planning and linkage.
[I]t’s disrespectful but it’s also just not very good for our community if GPs aren’t involved in the disaster management plan because disasters take, this is going to take, quite a few years to recover. (GP01)
GP integration into the wider response is slowly beginning. Guidelines are being developed. The recently developed HealthPathways disaster resource27 is one example of this. GP organisations are now providing resources to support basic planning and response.25,28–32 However, GPs currently need to initiate their own planning. Each practice needs to develop their own contextualised business continuity disaster plan for unpredicted local events. Linking to other local health providers and services – particularly pharmacies, emergency departments and other general practices – provides back-up support.
GPs can also play an important part in disaster healthcare preparedness for their patient population specific to their local context and health needs, including ensuring an up-to-date My Health Record. GPs can contribute to recovery with early identification and management of disaster health effects and ongoing surveillance for deterioration of chronic disease.
Disasters will always challenge comprehensive healthcare provision in the community, but integration of a well-prepared primary care response could be expected to improve patient healthcare, as well as the experience and safety of responding GPs during such difficult times.
By the time disaster strikes, it is too late to start planning.
Appendix A: Semi-structured interview – questions