Case
A woman aged 19 years sustained a minor puncture wound to her left inner thigh while travelling in remote outback Australia. Five hours after the initial injury, the patient developed symptoms of dizziness, nausea and disproportionately severe pain, associated with progressive swelling at the wound site. These symptoms worsened over 24 hours, and dusky discolouration developed around the wound (Figure 1). She presented to the emergency department in septicaemic shock with fever, tachycardia and hypotension. Empirical intravenous antibiotics and haemodynamic support were instituted; however, her condition continued to deteriorate over the next 24 hours. After referral to the local surgical team, surgical exploration was undertaken, during which gas was noted within the wound. A diagnosis of necrotising fasciitis (necrotising soft tissue infection [NSTI]) was made. The patient was transferred to a tertiary centre, where she underwent numerous serial surgical debridements of the subcutaneous tissue and underlying musculature (Figure 2), and when deemed clear of infection, extensive split skin grafting procedures (Figure 3).
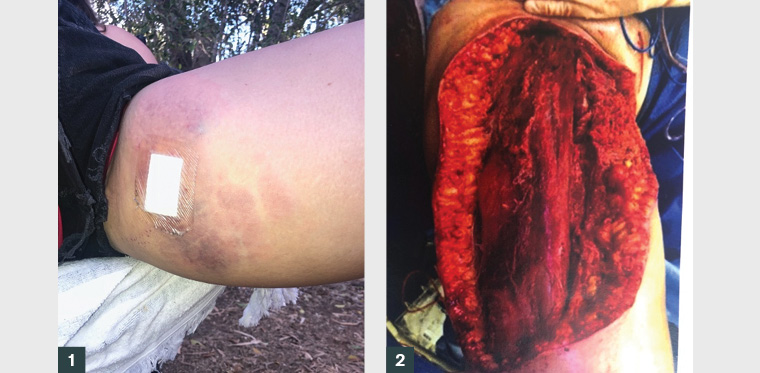
Figure 1. Evolving necrotising soft tissue infection
Figure 2. Surgical debridement
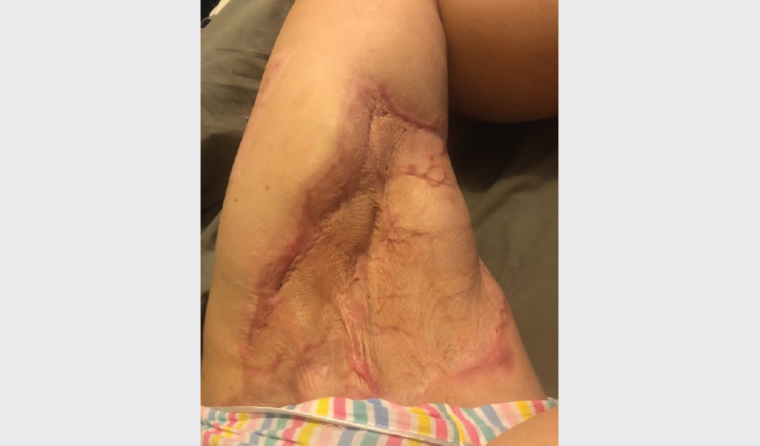
Figure 3. Grafting to defect site
Question 1
What are the red flags in this case that suggest the need to exclude NSTI, and what other differential diagnoses should be considered?
Question 2
Are there any risk factors for this condition?
Question 3
Which pathogens are responsible for NSTIs?
Question 4
What should management of NSTIs entail?
Question 5
What are some of the long-term complications that general practitioners may encounter following NSTIs?
Answer 1
NSTIs are rapidly progressive infections of the skin, fat, fascia and muscle, and they may result in advancing necrosis, sepsis, systemic shock and death.1,2 An NSTI is a clinical diagnosis; when suspected, urgent debridement should be performed.
The ‘triad’ of NSTI symptoms includes disproportionate local pain, swelling and erythema/skin changes.3 NSTI generally occurs after a trauma, either major or minor, but may be idiopathic.1 The highest-risk wounds are those that introduce bacteria to the deep tissue planes,4 such as puncture wounds or deep cuts. Additional symptoms may include flu-like symptoms5 such as fever, diarrhoea and general malaise, or dizziness and nausea as outlined in this case. These may progress to systemic signs including tachycardia, hypotension and altered mental state.1,4 Most commonly affected are the upper and lower extremities, abdomen and perineum.6
Clinicians should have a high index of suspicion for presentations of subcutaneous infection that seem ‘not quite right’.2 Early presentations can be difficult to diagnose because of limited initial signs.4 Initially, infections track along the deep fascia, and the extent of infection therefore may not be initially visually apparent.4 As NSTIs progress, the affected region will often swell and may develop a purpuric rash that is due to thrombosis of the perforating blood vessel that supplies that area of the skin (Figure 1). The thrombosis of these blood vessels may occur secondary to bacterial spread, and ischaemic tissue can result in necrosis, haemorrhagic bullae and ischaemia progressively in the affected regions.1,4 Crepitus may also occur, due to Clostridium species producing gas under the skin.7
Differential diagnoses based on localised signs include cellulitis, superficial abscesses, pyoderma gangrenosum, arterial insufficiency and compartment syndrome.4,8 Late NSTI may culminate in systemic shock,6 with other potential causes of shock to be considered as differentials. In this case, given the geographic location, it would be reasonable to consider melioidosis, as this may present acutely in at-risk patients.9
Answer 2
While young and well individuals may develop NSTI,4 any condition with the potential for lowered immunity confers increased risk (Box 1). Wounds that seed bacteria to the deep tissue planes carry increased risk,4 and hence appropriate washout of potentially contaminated wounds is particularly significant in NSTI prevention.
| Box 1. Risk factors for necrotising soft tissue infection4,6,13 |
- Diabetes (most frequent)
- Chronic disease
- Immunosuppression
- Obesity
- Malnutrition
- Peripheral vascular disease
- Intravenous drug use
- Underlying malignancy
- Elderly
- Aboriginal and Torres Strait Islander descent
- Chronic alcohol abuse
|
Answer 3
NSTIs may present as a polymicrobial or monomicrobial infection.
- Type 1 – Common organisms in polymicrobial infections: Streptococcus spp., Staphylococcus spp., Bacteroides spp. and Escherichia coli.3,10
- Type 2 – Monomicrobial presentations may include Staphylococcus aureus and Streptococcus pyogenes.6
- Type 3 – Marine bacteria may be causal organisms in marine environments.6
- Type 4 – Fungal species can also be causative in immunocompromised hosts.6
Answer 4
Surgery with major debridement is the key management strategy for NSTIs.2 Mortality rates are 20–40%.2 As such, high-risk cases should be immediately referred to hospital for surgical management.4 Initial management also includes immediate administration of broad-spectrum antibiotics in addition to supportive measures for comorbid shock and sepsis.4,6
Investigations (Table 1) should not delay definitive surgical treatment but may play an adjunct role in assessment, especially when the diagnosis is unclear.7 Where laboratory investigations are available, clinical scores for differentiation of NSTI may be applied, such as the Laboratory Risk Indicator for Necrotising Fasciitis (LRINEC) score. LRINEC assesses probability of NSTI through a point score system measuring laboratory markers of C-reactive protein, white cell count, haemoglobin and serum sodium, creatinine and glucose levels.4 An LRINEC score of ≥6 is suggestive of NSTI.11
| Table 1. Potential investigation findings in necrotising soft tissue infections1,4,6 |
| Test to consider |
Possible findings |
| Full blood examination |
Leucocytosis |
| Urea, electrolytes and creatinine |
Elevated creatinine, reduced estimated glomerular filtration rate, raised urea |
| Creatinine kinase |
May be elevated |
| C-reactive protein/erythrocyte sedimentation rate |
May be elevated |
| Serum lactate |
May be elevated |
| Blood gas |
May show metabolic acidosis |
| Coagulation studies |
May be anomalous |
| Blood cultures |
Can be positive and guide antibiotic choice |
| X-rays |
May show gas gangrene |
| Computed tomography, ultrasonography and/or magnetic resonance imaging |
May show soft tissue swelling and associated gas gangrene |
Answer 5
Individuals with NSTIs frequently require a prolonged hospital admission, often with a significant portion spent in an intensive care unit. Patients commonly undergo an extensive tissue resection, and they may be significantly deconditioned or encounter impairment due to complicated reconstructive plastic surgery. Survivors often endure a tumultuous journey of rehabilitation with physical, social and psychological sequelae.12
Case continued
For the patient in this case study, rehabilitation has been complex. At two years following the acute NSTI illness, chronic complications include recurrent graft breakdown and infection, ongoing reduced mobility and delayed return to work and study. The defect of her left thigh (Figure 4) has caused significant psychological morbidity, and her ultimate reconstructive strategy will involve complicated, multi-staged operations.
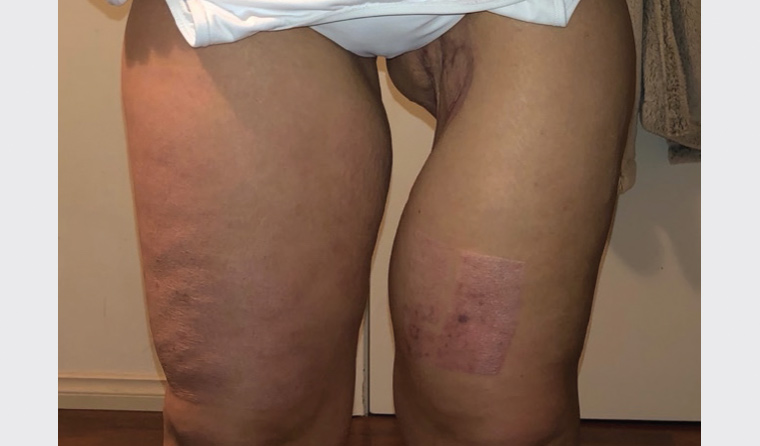
Figure 4. Post-surgical defect
Key points
- Careful attention to wound management with debridement of dead tissue is the key to preventing NTSI.
- Wounds at high risk of NSTI include injury in the immunocompromised, and wounds that introduce bacteria to the deep tissue planes.
- There must be high index of suspicion for presentations of soft tissue infection with disproportionate pain, systemic symptoms and haemodynamic compromise.
- An NSTI is a clinical diagnosis and requires urgent, definitive debridement, not imaging.