Case
A male aged 16 years presented to the emergency department with a three-day history of oral ulceration involving the lips (Figure 1) that was associated with skin (Figure 2) and genital lesions (Figure 3). These lesions occurred suddenly and concurrently. He was systemically unwell, with low-grade fevers and diminished oral intake. He had no significant medical history or medication use.
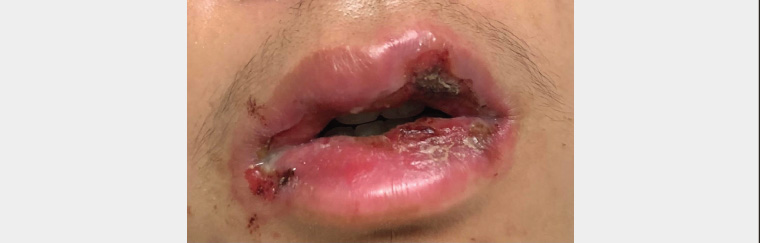
Figure 1. Crusting and ulceration of lips
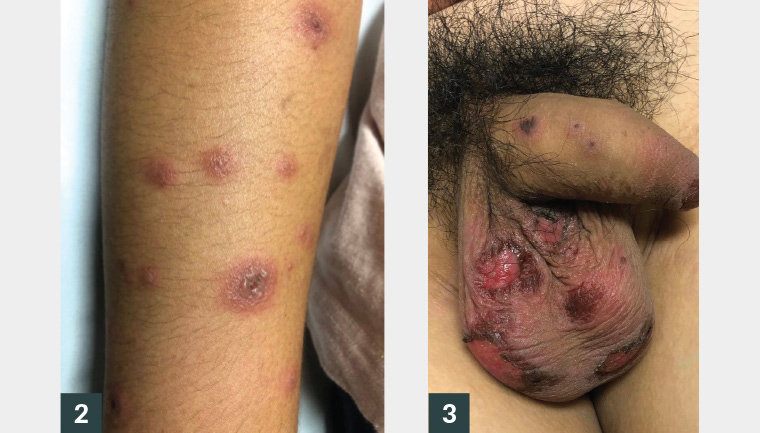
Figure 2. Targetoid lesions on patient’s arm
Figure 3. Erosions on scrotum and lesions on penis
Question 1
How would you describe the large lesion pictured on the skin (Figure 2)?
Question 2
What are the differentials associated with target lesions?
Question 3
What investigations are required when suspecting this condition?
Question 4
How is this condition treated, and when would a patient require hospitalisation for management?
Answer 1
Figure 2 shows a well-demarcated targetoid lesion with three concentric rings consisting of an outer erythematous ring, oedematous second ring and dusky crusted centre.
Answer 2
Typical target lesions such as those seen in this case (Figure 2) occur characteristically in erythema multiforme,1 which is an acute cutaneous hypersensitivity reaction; the skin lesions appear 48–72 hours after onset of the illness and favour the arms and legs. Mucosal surfaces such as the mouth and eyes can also be affected. When mucosal involvement is severe the condition is known as erythema multiforme major. It commonly occurs in young adults aged 20–30 years, and the lesions heal within 2–3 weeks in erythema multiforme minor and 4–6 weeks in erythema multiforme major. A major differential is Stevens–Johnson syndrome (SJS), which generally presents with macular target lesions that can rapidly progress to desquamating lesions. Erythema multiforme is most commonly precipitated by herpes simplex virus (HSV) infection2 and less commonly by mycoplasma infection. Medications can also trigger this condition, and these include penicillins, cephalosporins, macrolides and many others. There are various differentials of targetoid lesions, including the following non-exhaustive list:3
- SJS/toxic epidermal necrolysis (TEN): present with atypical target lesions that are purely macular (flat) and may only have two concentric rings.1 These target lesions progress rapidly to widespread epidermal desquamation with a total surface area of 10% in SJS and >30% in TEN.
- Fixed drug eruptions: can look like a plaque with a dusky centre and erythematous base and tend to re-occur on the same part of the body every time a specific causative drug is taken.
- Vasculitis: immunoglobulin (Ig) A vasculitis (Henoch–Schönlein purpura) and urticarial vasculitis can present with targetoid lesions.
- Subacute cutaneous lupus erythematosus: usually presents as annular lesions on photo-exposed areas but in some situations can form targetoid lesions (Rowell’s syndrome).
- Trauma: high-speed impact of objects onto the skin can produce a targetoid ecchymosis.
- Urticaria: can present as targetoid lesions with erythematous borders and central clearing; the main differentiating feature is the evanescent nature of urticaria, which, by definition, clears within 24 hours.
Answer 3
Erythema multiforme is a clinical diagnosis and does not necessarily require further investigation if history and examination are suggestive. Infections, such as HSV, are a common precipitant of erythema multiforme; therefore, serology may be beneficial in recurrent cases without evidence of previous HSV. Mycoplasma pneumoniae is also a known precipitant and can be investigated with respiratory swabs or chest X-ray if clinically indicated.4 Where the diagnosis is not entirely clear, skin biopsies can help differentiate between the potential causes.
Other precipitants are less common but can be considered in the absence of preceding infective symptoms. Some examples include medications, autoimmune conditions and malignancies.
Answer 4
Treatment is focused on simple skincare measures and symptomatic management. Soap-free washes and emollients are important to maintain healthy and well-hydrated skin. Pruritus can be treated with oral antihistamines. Oral care is focused on minimising pain with lignocaine 2% rinsing solution and emollient for the lips with white soft paraffin.
Erythema multiforme can usually be managed as an outpatient; however, hospitalisation may be required in the case of significantly reduced intake due to severe oral involvement. This can lead to dehydration, electrolyte disturbances and malnutrition. In this situation, systemic steroid therapy can be used (0.5–1 mg/kg of prednisone daily)
5 until systemic improvement, in addition to the aforementioned measures.
Case continued
The patient had poor oral intake for several days due to oral mucosal involvement and was admitted to hospital for intravenous fluids and systemic treatment with prednisone. He was treated symptomatically and required nasogastric tube feeding for two days while his oral mucous membranes recovered. He had positive HSV type 1 IgM serology, indicating that HSV infection was the likely precipitant for this eruption.
Question 5
What are the potential complications of this condition?
Question 6
How can this condition be managed if it recurs?
Answer 5
Ocular complications such as keratitis and visual impairment6 can be caused by erythema multiforme when the eyes are not examined for injection and oedema. In a situation in which ocular involvement is suspected, the patient should be referred for ophthalmological assessment. There is an uncommon variant of erythema multiforme that is difficult to diagnose known as erythema multiforme majus (Fuchs’ dystrophy),7 which mainly affects mucosal surfaces. Without characteristic skin lesions, such ocular complications may be missed. Other potential complications include scarring of the skin and strictures in the urethra and vagina where inflammatory lesions have healed. Generally, patients will recover without long-term issues.
Answer 6
Prophylactic therapy for recurrent erythema multiforme is not always required. Eliminating the precipitant, if known, can prevent recurrence altogether. In the setting of HSV-induced recurrent erythema multiforme (six or more episodes per year), prophylactic doses of antiviral therapy can be used (valaciclovir 500 mg daily or aciclovir 400 mg twice daily for six months). If therapy is ineffective, referral to a dermatologist may be required for consideration of alternative treatment options.
Key points
- Erythema multiforme is an acute hypersensitivity reaction that most commonly occurs secondary to HSV infections.
- Targetoid lesions with three concentric rings consisting of an outer erythematous ring, oedematous second ring and dusky crusted centre are characteristic of erythema multiforme.
- It is important to consider SJS and TEN when a patient presents with targetoid lesions – these conditions can have target lesions that rapidly desquamate and can be life threatening.
- Treatment of erythema multiforme is supportive with general skincare measures, antihistamines for pruritus, white soft paraffin for lip lesions and anaesthetic mouth gargle for oral lesions.