The term ‘pivot’, meaning a quick turnaround, evolved during the COVID-19 disruption to reference the rapid transition from face-to-face delivery of instructional opportunities to virtual and online alternatives.1–8 For some, the pivot was not viewed favourably due to the historical predominance of face-to-face offerings.9 Others assumed the shift from face to face would be easy; a view that does not accurately reflect the extensive effort put into creating viable alternatives necessitated by public health directives of mandated lockdowns, limited face-to-face interactions and social distancing.10 Nor does that view capture the time required for delivering flexible learning experiences and assessment in times of disruption.11
Pivoting to virtual supervisor continuing professional development: A case study
Eastern Victoria (EV) GP Training was one of the nine Australian registered training organisations (RTOs) providing training for Australian general practitioner (GP) training registrars and ongoing professional development to Fellowed GPs who are supervisors.12 To the end of 2022, when training reverted to the GP colleges, EV GP Training delivered education and training throughout eastern Victoria. Its broad training region covered eastern metropolitan Melbourne, the Mornington Peninsula and Gippsland (Figure 1). The organisation had two offices: one in Hawthorn (metropolitan Melbourne) and the other in Churchill (Gippsland). A significant component of EV GP Training’s role was delivering continuing professional development (CPD) to GP supervisors.
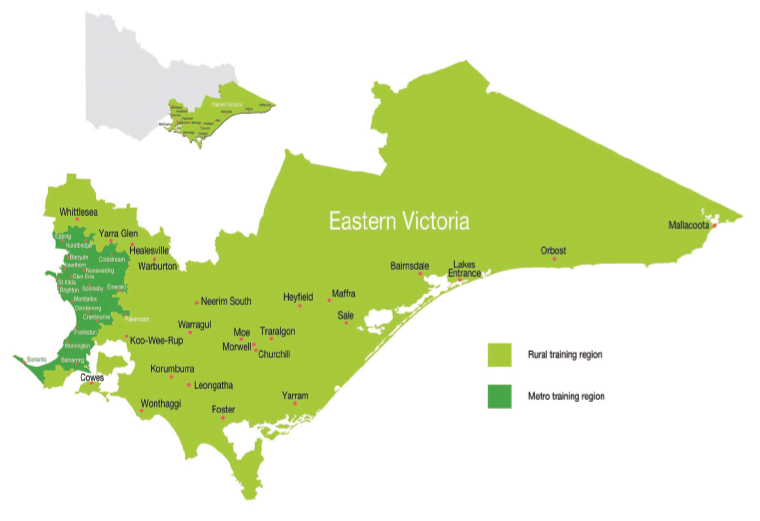
Figure 1. Eastern Victoria GP Training’s training region. Click here to enlarge
Reproduced from Eastern Victoria GP Training, with permission.32
Metro, metropolitan.
Knowledge is also socially constructed,13 built from mutually shared beliefs and embedded in practice.14 In professional training contexts, and from an andragogical perspective,15 adult learners benefit from opportunities to participate in communities of practice16–19 and the collective knowledge contained therein,20,21 participating through shared discussions.
In the training context, and prior to the COVID-19 pandemic, supervisor CPD at EV GP Training had been conceptualised as face-to-face delivery, with localised training at an RTO office or in hired venues across the region. However, supervisor post-session feedback at EV GP Training over the years had evidenced increasing requests for flexible delivery; despite these requests, concern was expressed from various key stakeholders that supervisors would not be able to engage with each other in virtual environments. The value placed on the face-to-face opportunities to connect had been seen historically as one of the strengths of the organisation.
As workplace trainers, GP supervisors complete compulsory annual educational CPD as an accreditation requirement for training registrars. There were specific programs for aspiring, new (in their first three years) and experienced (the largest group) supervisors. The number of aspiring and new supervisors varied each year depending on practice numbers and changes. In 2019, EV GP Training’s team conducted a CPD audit, identifying more than 500 supervisors in deficit. This was problematic: no CPD, no registrar and thus a GP workforce issue. A larger program of CPD was developed to meet this shortfall.
In 2020, the world faced the greatest challenge it has seen in recent times with the global COVID-19 pandemic. When lockdowns were imposed across the state of Victoria, Australia, participating supervisors, facilitators (including medical educators) and RTO staff were all affected and alternative modes of CPD delivery re-entered senior management discussions.
The entire 2020 supervisor professional development program, which had been prepared for face-to-face satellite learning across EV GP Training’s broad geographical footprint, had to shift to virtual participation overnight. The shift in the conceptualisation of virtual delivery of supervisor professional development at EV GP Training ushered in many associated and unfamiliar challenges.
At the time, the RTO had in its employ a manager of supervisor professional development who had a background in medical education and was acknowledged by peers to be an expert in open, blended, distance and flexible learning.22 Adopting the notion of ‘elastic practice’,23 multiple theoretical bases were integrated in adaptive, responsive approaches to practice, through a professional ‘toolkit’ of techniques, experiences and ideas, curated over a career in educational development. This enabled the rapid development and deployment of seven strategies to meet CPD needs and engage learners.
Seven strategies for the pivot
First, although EV GP Training’s learning management system (LMS) was regularly used for registrar training, it had not been used for supervisor CPD. A structure was developed for pre-accredited, new and experienced supervisors, resources and related assessments. This required instruction for supervisors, achieved through the LMS familiarisation at the commencement of every CPD session between March 2020 and December 2021; how to locate the LMS on the EV GP Training intranet, how to log in and access the content.
Second, with regard to videoconferencing, one of the team had successfully trialled the use of videoconferencing for education and CPD for an Australian university in 2014, so in pivoting to synchronous (live) online delivery, it was adopted for the Supervisor CPD, making extensive work of the breakout rooms for small group learning. There was much work to be done initially to instruct session facilitators in the affordances of the technology, pedagogy (eg using online role play for engagement, different possibilities for the breakout rooms), participant engagement and videoconferencing etiquette. In addition, there was a moderator for all events, who often acted as a facilitator at times when the main facilitator’s Wi-Fi dropped out. Participant engagement was fostered through a variety of options of the videoconferencing environment. Early learnings included the need for technical support for participants (commencing 30 minutes ahead and lasting 30 minutes into the session), administrative support to capture attendance (first 30 minutes) and session design (not scheduling complex breakout room role play pairings of experienced and less-experienced supervisors too close to the session start).
Third, asynchronous online alternatives for four core modules (undertaken anytime, anywhere in a given timeframe and for self-enrolment via the LMS) were developed with eLearning course development software. Based on the principles of effective instructional design, formative and summative assessment was incorporated into the learning design.24 Module evaluation was embedded for quality assurance purposes. Although rolled out across 2021, uptake was initially slow despite interest. On investigation, the issue was supervisors remembering their log-in details. LMS analytics were used to determine those who had not logged into the system, subsequently contacting them to provide their log-in details.
Fourth, blended modality was adopted to redevelop the full-day pre-accreditation workshop. These ‘foundation’ modules were a combination of online and live offerings. Module 1, on planning orientation for registrars, could be completed online asynchronously; Modules 2 and 3 (educational supervision, providing feedback, assessing competence and safety) were delivered as back-to-back 90-min live videoconferencing sessions; and Module 4, for review and assessment, was completed asynchronously online within two weeks after completion of Module 3. According to feedback, the benefits for busy clinicians included that they were only away from their clinic for a half day to participate in the live CPD.
Fifth, the main annual supervisor CPD event was rapidly pivoted to a multistreamed videoconferencing event: a massive undertaking because, traditionally, these two-day face-to-face residential workshops were held at large venues in metropolitan and regional locations and highly valued as networking opportunities. Using a flipped modality, pre- and post-work took place in the LMS. Feedback to the participant’s pre-work was integrated into the live sessions as conversation points. Feedback on the final assessment (participant self-reflection on how the participant intended to integrate their learning into practice) was provided to the individual by educators and clinicians, often suggesting other ideas for ways to adopt strategies in small and sustainable ways. Developing an online program that was attractive, gave frequent breaks to prevent screen fatigue and provided social spaces to meet virtually was key to success. Although not face-to-face, it provided a space for frontline healthcare professionals to network safely.
Sixth, evaluation of assessment tasks required revamping. In line with a variety of options to complete CPD hours, options were introduced for supervisors to review a selection of targeted education modules created by General Practice Supervision Australia. The self-reflective assessment of learning asked participants:
- to describe the alternative learning activity
- the key learning points from this activity and, as workplace trainers, to provide examples of activities the supervisor would use to build a teaching session for the registrar around this learning
- how this learning was implemented in registrar teaching and/or to provide a consideration as to what might be some of the challenges in delivering this session to registrars
- for their/their registrar’s reflections and/or feedback on how this went, including strategies to overcome any barriers
- to provide any other comments/feedback in relation to this activity.
For assessment parity, we co-developed a marking rubric around the activity. The structure used three levels (above, at or below), with opportunity for additional comments. An example of how the various responses might look in the rubric was also developed for assessors.
Finally, we addressed the dwindling CPD session feedback. Evaluation questions related to learning outcomes, learning needs, relevance to practice and participatory barriers in the CPD (participation completion rates were declining). Event feedback evolved from paper copy (2018) to an online survey (2019) to the innovative use of QR codes (mid-2020 onwards). QR codes to anonymous survey links were placed on the penultimate PowerPoint slide in each session, ahead of the ‘Thank you; Questions’ slide, allowing participants five-minutes’ completion time. The integration of the QR codes lifted feedback completion rates from below 50% to consistently greater than 80%. It was satisfying over the months to observe the videoconferencing audience hold their telephones up to the screen to access the feedback link on that penultimate slide. Sessions were iteratively refined based on this session feedback. Initially, we received feedback requesting more out-of-hours sessions, which we swiftly adopted. Later feedback revealed concerns that this new CPD flexibility would be lost in post-COVID training.
Discussion: A cautionary tale of limitations and lessons learned
In shifting from place to space, there are important lessons to be shared. The urgent need for CPD opportunities led to the rapid pivot from face-to-face, place-based learning to teaching live (synchronously) via videoconferencing, fully online (asynchronously) and blended hybrid modality. This required massive change management provisions not only for the learners (supervisors in this context), but also for staff at the RTO (session facilitators and program support staff). Yet, between March 2020 and December 2021, most of the RTO’s supervisors were able to catch up on their professional development requirements. We shared these learnings at national education conferences and were able to integrate them into the national supervisor curriculum and framework development that EV GP Training led.
Hiatt’s ADKAR model for organisational change25 emphasises the consideration of the needs of the individual in the process (in this case, educational change) through five lenses:
- Awareness of the need for change
- Desire to participate in and support the change
- Knowledge necessary for change
- Ability to implement required skills and behaviours
- Reinforcement to sustain the change.
Reflecting on these principles, we had the Awareness and Desire, but our challenges related to the Knowledge, Ability and Reinforcement (K-A-R) parts of the acronym. We did well on focusing on the technical knowledge necessary to implement change, but had less time to consider the K-A-R component in the rapid deployment. The takeaway message is that it is hard to apply change management on the run.
Issues such as accessibility, diversity in skills or access to equipment and software, including necessary upgrades, and internet activity are all enablers to learning. This process is compounded, however, when staff are geographically dispersed across a state.
These limitations for pivoting to virtual learning fall into four main themes of skills, resources, organisational strategies and support, and attitudes.26 A fifth theme may be added: that of social connectedness. Enhancing opportunities for virtual social connections in times of disruption are vital. Challenges to pivoting online and their solutions are presented in Table 1 (overleaf).27–29
| Table 1. Challenges and solutions in pivoting online |
| Area |
Challenges |
Solutions |
| Skills |
- Users not reading instructions due to time-pressures, or not being able to recall the information on how to use technology at a later time.
|
- Upskilling staff, including supporting willingness to upskill
- Upskilling users, including the provision of support at session starts and targeted communication
|
| Resources |
| Time |
- Time required in reformatting to virtual delivery
- May not be able to get through what you can in a face-to-face session
|
- Learning what can and cannot be achieved online versus face to face, what length of time audiences will engage over and whether the same content can be delivered in the same timeframe as face to face
|
| Technology |
- Disruption and disengagement in using the technology
- Different participant devices
- Different participant skill capability
|
- Establish participation etiquette in using the technology from the outset and reinforce
- Modelling by facilitators on how to use systems such as ‘chat’ in videoconferencing
|
| Internet, hardware and software issues |
- Internet and network connectivity27 and unreliability and unpredictability can be barriers in participation for both learners and facilitators
|
- Reinforce that internet issues of the end-user are not the facilitator’s/moderator’s/support staff’s issue
- However, ensure back-up plans and contingencies
|
| Organisational strategies and support: Back-channel communications |
- Facilitator’s connectivity and dropping out
|
- Set up back-channel communications early to enable communications between key personnel
- This allows resolution of issues without disrupting the flow of session delivery
|
| Attitudes |
- Disruptive innovations might create complex problems,28 including stakeholder unfamiliarity or discomfort with some of the ways in which teaching, and learning, is disrupted29
- The importance of promoting confidence in the software/learning tool
- Change management as we shift from predominantly face to face to a blended learning model
|
- Consider ways to engage the digitally ‘absent’ or disengaged learner
- Scaffold and reinforce the changes
- Promote the positive; work towards minimising the barriers
|
| Social connectedness and engagement |
| Social connections |
- Lack of social connections in both synchronous and asynchronous learning opportunities
|
- To foster social connections, considering ways to connect and engage with others via the available technology in both synchronous and asynchronous manners is crucial in discussions and in the evolution of the learning design
|
| Active engagement |
- A lack of active engagement leads to non-participating learners
|
- Fostering active engagement includes:
- Enabling small group discussions such as via breakout rooms
- Enabling agency of leadership in facilitating a small group and summarising the adult learners’ insights to present back to the plenary on behalf of the small group
- Using polling functionality to create an expectation of engaging with content and providing responses
- Using emojis and the chat function to gauge learner feelings and experience
|
Conclusion
There is no doubt that the global pandemic changed how we conceive and deliver education. These conversations are echoing around undergraduate, graduate and prevocational medical training.30,31 Hybrid and online modalities, once considered in some circles to be the ‘poor cousin’ of face-to-face training, are now mainstream; a recalibration has taken place. Assisting this transition is crucial in training considerations as we move forward.
There are many barriers and enablers to providing CPD and building and maintaining a community of practice in times of change or disruption. Online and virtual learning opportunities are not fail-safe solutions. While providing equitable access on the one hand, on the other hand there are considerations around adult learning preferences, accessibility, diversity in skills or access to equipment and software, including necessary upgrades, and internet activity.
Educators also need to consider ways to engage the digitally absent or disengaged learner online or mitigate the intrusions of the disruptive learner or late arrival. Although educators might have many strategies in their professional toolkit of techniques,23 what works in face-to-face contexts might not work in the virtual world. However, with self-reflection plus group debriefing on aspects that did not work so well, and careful consideration of the learners and the context, alternative strategies can be trialled.
Success stories that rise above the obstacles warrant showcasing to encourage others facing similar circumstances. This includes making use of what is at hand to facilitate quality teaching, learning, feedback and assessment, despite disruptive changes. It also requires the sharing of ways in which social connectedness can be fostered when geographical collocation is not possible. The emerging literature supports our documented experiences.10 We carry these learnings into current roles.
Key points
- CPD is required to continually refresh knowledge, skills and attitudes towards professional practice.
- COVID-19 was a disruptor for traditional face-to-face delivery of CPD in many organisations around the globe.
- CPD quickly pivoted to virtual solutions; not all providers were equipped to face the challenge.
- Barriers to virtual CPD included rapid change management, upskilling all staff and students involved in delivery, maintaining social connectedness and handling technical issues. Opportunities included teamwork, thinking beyond the box for flexible solutions, enhancement of social connectedness and participant agency in learning.
- Lessons learned point to sustainable teaching options for future disruptions.