Case
A healthy man, aged 44 years, presented to a tertiary hospital with a one-week history of a painful eruption involving the right shoulder. The patient believed that the rash was a result of a burn injury caused by applying a hot water bottle to relieve neck pain, which preceded the development of the rash. He was assessed by his general practitioner who provided analgesia and silver sulfadiazine cream. However, the cutaneous involvement progressed. Four days later, the affected area evolved into a pustular eruption (Figure 1, 2) associated with severe pain. The patient remained systemically well. He was immunocompetent with no significant medical history, medication use or known allergies. Routine investigations were within normal limits except for an elevated C-reactive protein of 66 mg/L.
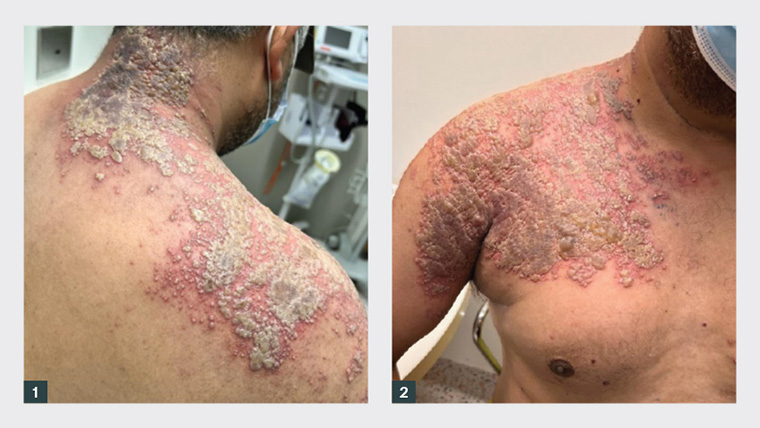
Figure 1. Posterior view of the pustular eruption of the right shoulder.
Figure 2. Anterior view of the pustular eruption of the right shoulder.
Question 1
Describe the lesion in Figures 1 and 2.
Question 2
What is the most likely diagnosis? What are the other differentials to consider?
Answer 1
Both figures demonstrate confluent and coalescing pustules with associated crusting on an erythematous base in a dermatomal distribution involving the right posterior base of the neck, right shoulder and anterior chest.
Answer 2
A painful vesiculopustular eruption might occur in herpes zoster, commonly known as shingles, a viral syndrome due to reactivation of dormant varicella zoster virus (VZV). The rash appears over 3–5 days after a prodrome of fever and burning pain. The lesions are unilateral and distributed within a single dermatome.1 A major differential is herpes simplex virus type 1 (HSV-1) infection, which characteristically manifests as a painful vesicular rash in the same dermatome where it was inoculated into the skin. It commonly affects the face and mucosa but can become disseminated in immunocompromised individuals and in those with underlying dermatological conditions such as atopic dermatitis (eczema herpeticum) and Darier’s disease. Other differential diagnoses to consider are acute localised exanthematous pustulosis (ALEP) and evolving acute generalised exanthematous pustulosis (AGEP). These are cutaneous adverse drug reactions characterised by an eruption of sterile pustules typically following drug administration.2,3 Both ALEP and AGEP highlight the importance of obtaining a medication history, as antibiotics and non-steroidal anti-inflammatories, for instance, have been commonly implicated in these cases. It is also essential to consider secondary bacterial infection as a differential diagnosis, especially when a history of skin injury or trauma is elicited. Finally, an atypical presentation of pustular psoriasis, localised or koebnerised, is also important to consider in a pustular eruption, albeit in this case, the striking dermatomal distribution makes this less likely.
Question 3
What investigations would you perform?
Question 4
What is the treatment of choice for this condition?
Answer 3
An accurate diagnosis of herpes zoster can be made from history and clinical examination due to its distinctive presentation. However, laboratory testing can be useful to confirm diagnosis and to identify the responsible virus. This is necessary, as advice to avoid pregnant women is essential for individuals with herpes zoster virus, and the dosing of antiviral therapy is higher for herpes zoster than for HSV-1. Polymerase chain reaction (PCR) is most useful for confirming a clinical suspicion of herpes zoster due to its high sensitivity and rapid turnaround time. Bacterial swabs for microscopy, culture and sensitivity (MCS) are important to exclude bacterial infection and secondary bacterial infection, which are common in herpes zoster infection. Additionally, skin biopsy might be needed to exclude other differential diagnoses of an inflammatory aetiology, such as a drug eruption and pustular psoriasis.
Answer 4
Antiviral therapy is used to reduce the severity of illness and accelerate the resolution of pain and skin lesions. It is most effective when initiated within 72 hours of rash onset. Additionally, early treatment reduces the risk of developing complications such as postherpetic neuralgia (PHN) and is especially important in elderly people, who have a higher risk of PHN. Current Australian guidelines recommend famciclovir and valaciclovir, as they have greater bioavailability and simpler dosing regimens compared to aciclovir. The dose for valaciclovir is 1 g three times daily for seven days.4
Case continued
Viral and bacterial swabs for PCR and MCS were performed, and the patient was commenced on valaciclovir 1 g three times daily for seven days. Advice on the natural course of VZV infection was given, including on potential complications such as postherpetic neuralgia. Education on transmission prevention of the virus was provided, and the patient was advised to minimise exposure to family members, vulnerable individuals such as pregnant women and those who are immunocompromised or with no previous varicella immunisation.
Question 5
What is the most frequent complication of herpes zoster? How should it be treated?
Question 6
How can this condition be prevented?
Answer 5
PHN is defined as pain persistent for more than four months after the onset of the rash. This differs from usual herpes zoster pain, which lasts two to four weeks. Current guidelines recommend oral therapies such as tricyclic antidepressants, gabapentin, pregabalin and opioids as well as topical lidocaine and capsaicin patches for the treatment of PHN.5 While both have been shown to provide effective analgesia, oral therapies are associated with systemic adverse effects.5 Additionally, 2% of pregnant women exposed to herpes zoster virus in the first 20 weeks will develop foetal varicella syndrome.6 VZV immunoglobulin is a possible treatment, and consultation with foetal medicine or infectious diseases should be considered, preferably within 72 hours of exposure.6
Answer 6
It is important to vaccinate susceptible individuals to prevent shingles. There have been recent changes to the National Immunisation Program that have made available a two-dose course of Shingrix for people aged 65 years or older, First Nations people over 50 years of age and immunocompromised patients over 18 years of age. Shingrix does not contain live virus and has been found to be more effective than older vaccines (eg Zostavax).7 This is significant because it can be safely given to immunocompromised people.7 Specialist advice is recommended according to individual circumstances.
Key points
- Pustular eruptions have a wide differential diagnosis.
- Herpes zoster (shingles) can be diagnosed clinically; however, a VZV PCR swab is prudent to confirm infectious aetiology.
- Oral valaciclovir 1 g three times daily for seven days is usually the treatment of choice.
- The new Shingrix vaccine is more effective than Zostavax, and it should be offered to people aged 65 years or older, First Nations people over 50 years of age and immunocompromised patients over 18 years of age.