Case
A girl, aged 17 years, of Korean descent presented with a three-day history of fever, malaise and skin pain, and a one-day history of mucocutaneous blisters. The patient had a history of borderline personality disorder and major depression and had been prescribed lamotrigine by her psychiatrist two weeks before the presentation. She also reported daily use of tobacco and cannabis, and the occasional use of amphetamine.
On examination, the patient had blisters arising from dusky red plaques on bilateral cheeks, yellow crusts and erosions on her lips and widespread macular atypical targets on the body and limbs (Figure 1). Nikolsky’s sign, characterised by the detachment of healthy skin upon lateral pressure, was positive.
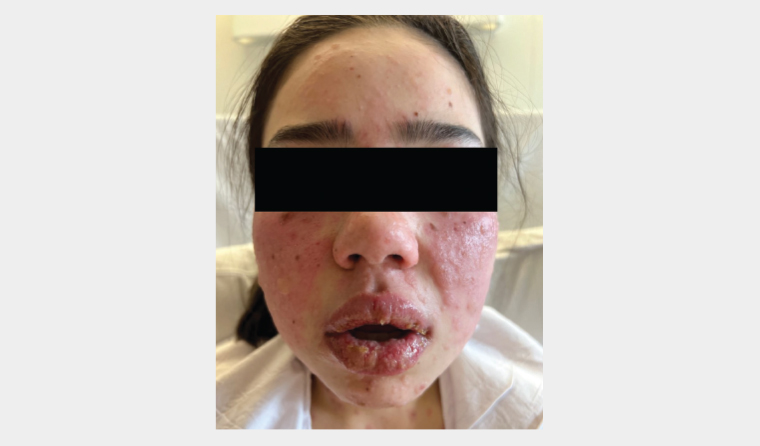
Figure 1. Multiple blisters arising from the dusky red papules and plaques on bilateral cheeks. Blisters, crusting and erosions are also present on the lips.
Question 1
What are the potential differential diagnoses?
Answer 1
A positive Nikolsky’s sign is indicative of compromised structural integrity within the epidermal layer. This sign has been observed in many dermatological conditions, including Stevens–Johnson syndrome (SJS)/toxic epidermal necrolysis (TEN), autoimmune blistering diseases and staphylococcal scalded skin syndrome.1 Erythema multiforme, Mycoplasma pneumoniae-induced rash and mucositis and TEN-like lupus erythematosus are also potential differential diagnoses (Table 1).
| Table 1. Differential diagnoses |
| Disorder |
Aetiology |
Clinical features |
| SJS/TEN |
Drug reaction |
- Prodromal illness one to three days prior to cutaneous manifestation
- Skin tenderness, dusky red macules and patches, blisters and mucositis
|
| EM |
Infection in 90% of cases |
- Often precipitated by herpes simplex virus
- Typical targets on skin and severe mucosal involvement in EM major
|
| SSSS |
Exfoliative toxins released by Staphylococcus aureus |
- Mainly affects children aged <5 years
- Prodrome of malaise, fever, irritability and tenderness of the skin
- Extensive erythema with skin desquamation
|
| MIRM |
Mycoplasma pneumoniae infection |
- Mainly affects children
- Significant mucositis with absent to sparse cutaneous involvement
|
| TEN-like lupus erythematosus |
Autoimmune |
- Acute lupus erythematosus present with clinical features similar to TEN
|
| Pemphigus |
Autoimmune |
- Flaccid vesicles and erosions
|
| Pemphigoid |
Autoimmune |
- Tense vesicles and blisters
|
| EM, erythema multiforme; MIRM, Mycoplasma pneumoniae-induced rash and mucositis; SJS, Stevens–Johnson syndrome; SSSS, staphylococcal skin scalded syndrome; TEN, toxic epidermal necrolysis. |
Case continued
The patient was lymphopenic (0.64×109/L; reference interval [RI] 0.9–3.30×109/L) with elevated C-reactive protein (31 mg/L; RI 0–5 mg/L). Liver function and urea electrolytes and creatinine were normal. Septic screens were negative.
Histopathological examination showed extensive full-thickness epidermal necrosis with scant perivascular lymphocytic infiltrates. Direct immunofluorescence was negative.
Question 2
What is the most likely diagnosis?
Question 3
What is SJS/TEN?
Answer 2
The findings are consistent with SJS/TEN. SJS/TEN usually begins with a prodromal illness, characterised by fever, malaise and upper respiratory tract symptoms, followed by cutaneous manifestations such as dusky red macules, patches, blisters and mucositis, along with a positive Nikolsky’s sign. Systemic manifestations, such as fever, lymphadenopathy, hepatitis, cytopenias and cholestasis, might also occur.2
Answer 3
SJS/TEN is a rare, severe and potentially fatal hypersensitivity reaction characterised by epidermal necrosis leading to blistering and skin loss. It is differentiated based on body surface area (BSA) involvement: SJS, <10%; TEN, >30%; and SJS/TEN overlap, 10–30%. The pathogenesis remains unclear; an immune-mediated reaction against keratinocytes resulting in apoptosis has been proposed.2 Medications, including sulfonamide antibiotics, anti-epileptic drugs, allopurinol and oxicam non-steroidal anti-inflammatory drugs, are common triggers.2
The mortality rate ranges from 10% to 50% depending on disease severity, patient comorbidities and the standard of care of patients.3 Complications from the loss of skin barrier function, such as hypovolaemia, electrolyte imbalance, renal insufficiency and sepsis, are the main causes of mortality.3
Case continued
The patient was immediately transferred to a burns unit for multidisciplinary care. She was managed with topical greasy emollient, intravenous immunoglobulin (IVIG), cyclosporine, etanercept and analgesia. Despite treatment, she progressed to TEN with 60% BSA involvement (Figure 2). The patient fortunately made a complete recovery and was discharged home after three weeks of hospital admission.
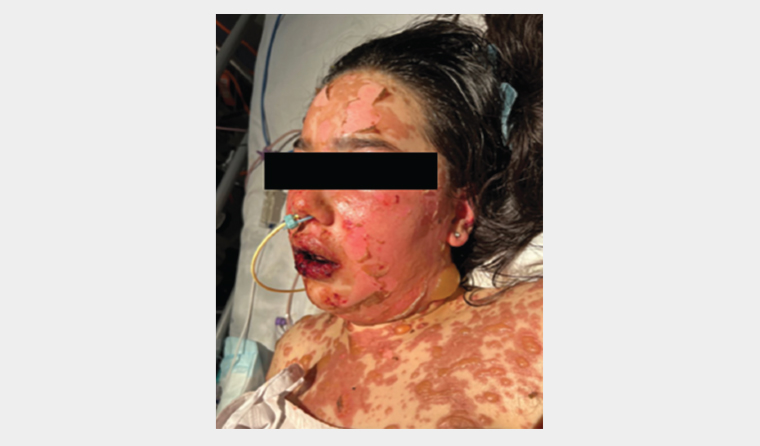
Figure 2. Day 5 of hospital admission. There is significant cutaneous desquamation and blistering on the face, neck and chest, along with severe haemorrhagic crusting on the lips. A nasogastric tube was inserted because the patient was unable to tolerate oral intake due to pain.
Question 4
What is the management of SJS/TEN?
Question 5
Can SJS/TEN be prevented?
Answer 4
A patient who is suspected to have SJS/TEN requires an urgent referral to the emergency department for further evaluation. The patient might be transferred to a specialised burns unit for supportive care in consultation with the dermatology team. A systematic review has shown that an early transfer to a burns unit and prompt discontinuation of the offending medication improve prognosis.4 General practitioners (GPs) might encounter these patients, particularly early in the disease course. Given GPs’ intimate knowledge of their patients’ medication history, they are well-positioned to make a diagnosis and identify the causative agent.
The medical treatment for SJS/TEN is largely supportive and aims to prevent complications. Systemic corticosteroid, IVIG, cyclosporine and etanercept might improve survival, but the data are limited to retrospective case series.5 The management details are beyond the scope of this article and there are published guidelines for those who are interested in this topic.6
Answer 5
The offending medication must be avoided in the future to prevent a recurrence. This requires a multifaceted approach that includes patient education, clear documentation, prompt communication with the patient’s GP and careful evaluation for potential cross-reactivity with the causative agent prior to prescribing any new medication.
In addition, pretreatment genetic screening of high-risk patients can prevent SJS/TEN. Certain human leukocyte antigen (HLA) types have been associated with an increased risk of SJS/TEN (Table 2).3,7,8 Some countries have implemented testing for HLA-B*1502 in individuals of Asian descent, successfully reducing the incidence of carbamazepine-induced SJS/TEN.7 The test is available in Australia, but is not currently subsidised (except in Victoria), costing around $80.8 Given the high mortality and morbidity of SJS/TEN, the test should be considered when prescribing high-risk medications in the at-risk population.9
| Table 2. Medication and gene variants that increase the risks of developing severe cutaneous adverse reaction in different populations6,7 |
| Medication |
Gene variants involved in medication exposure |
| Abacavir |
HLA-B*5701 |
| Allopurinol |
HLA-B*5801 in Han Chinese populations |
| Carbamazepine |
HLA-B*1502 in Han Chinese and South-east Asian populations
HLA-B*3101 in Japanese and Europeans populations |
| Lamotrigine |
HLA-B*1502 Han Chinese and South-east Asian populations
HLA-B*4403 |
Key points
- Patients who are suspected to have SJS/TEN require an urgent referral to hospital.
- Medication, such as carbamazepine, allopurinol and lamotrigine, is the most common trigger of SJS/TEN.
- Genetic testing is a useful tool to prevent SJS/TEN.